 |
 |
- Search
| Obstet Gynecol Sci > Volume 66(2); 2023 > Article |
|
Abstract
Objective
The study was conducted to determine the frequency of alloimmunization to various blood group antibodies in pregnant women, and the risk of hemolytic disease in the fetus and newborn.
Methods
All antenatal women, irrespective of the period of gestation or obstetric history, were included, whereas those taking anti-D immune-prophylaxis or with a history of blood transfusion were excluded. Antibody screening and identification were performed using a Bio-Rad ID microtyping system.
Results
Of 2,084 antenatal females, 1,765 were D-antigen positive and 319 D-antigen negative. Sixty-five (3.119%) women alloimmunized. Out of 54 (2.591%) who had sensitized to D-antigen, 11 (0.527%) also sensitized to other antibodies. These 11 alloantibodies identified included: anti-M (n=6; 9.23%), anti-C (n=1; 3.076%), anti-E (n=1; 1.538%), anti-e (n=1; 1.538%), anti-Lewis (a) (n=1; 1.538%), and unspecified antibodies (n=1; 1.538%). Multiple antibodies were seen in four patients that combined: anti-D and anti-C (n=2; 3.076%), anti-e and anti-c (n=1; 1.538%), and anti-D and anti-G (n=1; 1.538%).
Conclusion
The rate of alloimmunization in D-antigen-negative women was high. Apart from this, the alloimmunization rate in women with bad obstetric history was very high, at 8.1%. In developing countries such as India, universal antenatal antibody screening, though desirable, may not be justified at present, as the cost and infrastructure required would be immense because of the lower alloimmunization rates in RhD antigen-positive women. However, it is necessary to impose properly formulated protocols to screen pregnant women with bad obstetric history.
Even more than half a century after the advent of RhD prophylaxis, red cell alloimmunization still poses challenges to obstetricians [1]. This alloimmunization can lead to hemolytic disease of the fetus and newborn (HDFN). Other red cell antigens, namely C, c, E, and e, have also emerged as important causes of alloimmunization [1]. There are approximately 270 antibodies against red blood cell antigens [2]. The anti-A and anti-B antibodies against red blood cells are part of every adult immune system and thus are natural antibodies [3]. Any antibodies against red cell antigens other than anti-A and anti-B are considered unexpected, and can be either alloantibodies or autoantibodies. In pregnant women, such antibodies may cross the placenta and cause HDFN [2,4]. Untreated HDFN can cause neonatal mortality in up to 50% of cases [5]. Timely detection of such antibodies in antenatal women is essential for the early and better management of HDFN, and for the transfusion safety of the mother.
The alloimmunization rate varies from 0.4% to 2.7% among pregnant women worldwide [6]. There are only few studies from India that have studied alloimmunization in pregnancy. The alloantibody prevalence in India was found to be 1.25% in a study by Pahuja et al. [6]. In that study, the prevalence of alloimmunization was higher (5.5%) in pregnant women with bad obstetric history (BOH) than in normal pregnancies (0.5%). The issue of whether routine antibody screening in Rh-positive women is warranted, especially in developing countries like India, is still debated. The American College of Obstetricians and Gynecologists recommends routine antenatal testing at the blood bank for maternal blood type (ABO), RhD, and indirect antiglobulin test (IAT) for all pregnant mothers at the first antenatal visit, and additional antibody test at around 28 weeks in RhD negative mothers, whereas the United Kingdom recommends routine antenatal screening test at the blood bank for maternal blood type (ABO), RhD, and IAT for all pregnant mothers at the first antenatal visit, and at around 28 weeks for all mothers [7,8]. In India, according to the guidelines of the Directorate General of Health Sciences Technical Manual, Government of India, alloantibody screening is reserved for Rh-negative women or those with adverse obstetric history [1]. The studies from New Delhi, Tamil Nadu, Karnataka, and Andhra Pradesh have reported the frequency of these unexpected antibodies as 1.25%, 1.5%, 2.27%, and 1.1%, respectively [3,6,9,10]. However, no such reports are available for Western India (Rajasthan). Therefore, we aimed to determine the frequency of alloimmunization in Western India, and its outcome.
The detection of maternal alloimmunization against red cell antigens is vital for the management of HDFN. This was a prospective observational study conducted in the Department of Obstetrics and Gynecology in collaboration with the Department of Transfusion Medicine and Blood Bank, in order to measure the presence of alloimmunization to red cell antigens in antenatal women attending the antenatal clinic (ANC) of the apex tertiary care center of Western India, and to observe the proportion of minor blood group antibodies to assess the benefit of screening for those.
The main objectives of this study were to determine the frequency of alloimmunization to various blood group antibodies in pregnant women, and to determine the risk of HDFN in the Indian population.
All antenatal women registered in the Department of Obstetrics and Gynecology, All India Institute of Medical Sciences Jodhpur (AIIMS), India, for a period of 1.5 years were included in the study. Antenatal patients were screened for irregular antibodies using a commercial 3-cell antibody-screening panel during their first visit, irrespective of their gestation and parity. Antibody identification was performed on positive samples using a commercial 11-cell identification panel. Women who had received anti-D prophylaxis and blood transfusion in their current pregnancy were not included in the study.
With prior approval from the All India Institute of Medical Sciences (IEC/2018/800) Scientific and Ethical Committee and informed consent obtained from each patient, the name, age, sex, obstetric history, blood group, husband’s blood group (wherever possible), and history of blood transfusions were recorded before taking the blood samples. Blood samples were routinely collected at the booking visit and sent to the blood bank for ABO blood grouping. Additionally, RhD typing screened each of these samples for irregular antibodies by the Indirect Coombs Test, using a commercial 3-cell antibody screening panel [ID-DiaCell I-11-111]. Antibody identification was performed on samples that were found to be positive on the above screen, using a commercial 11-cell antibody identification panel [ID-DiaCell 1-11].
Blood samples (3 mL) were collected in ethylenediamine tetraacetic acid vacutainers and plain vacutainers which are allowed to clot, and centrifuged to separate the serum from the red cells. A 3% red blood cell suspension in saline was prepared and used for blood grouping and Rh typing according to laboratory protocols. ABO and Rh typing were performed by the Tube technique using commercial monoclonal -A, -B, and -D antisera (Tulip). The classification of blood groups was based on both forward and reverse grouping, and a negative control result. Testing for weak D (Du) was performed in all cases found to be D negative. Females were labelled as D negative only when the Du test result was negative. Antibody screening and identification were performed using the column agglutination technology in Coomb’s phase and a low ionic strength solution enhancer, according to the manufacturer’s instructions (DiaMed ID micro typing system; Bio-Rad, Cressier, Switzerland). Antibody screening was performed using a 3-cell screening panel, whereas identification was done using an 11-cell panel. Auto control was included in each test. A negative reaction (red blood cells pellets at the bottom of the microtube with no aggregates in the gel matrix) indicated the absence of detectable irregular antibodies in the patient’s serum or plasma. A positive reaction (a clear red line on the surface of the gel or agglutinates dispersed in the gel) indicated the presence of irregular antibodies. Positive results were graded from 1+ to 4+. Following the reaction pattern and red cell phenotyping, the type of antibody present was identified (auto control must be negative). Antibodies were characterized as non-specific if they did not fit into any of the reaction patterns, or if they reacted with all panel cells in the presence of a negative auto control. Serum samples positive for antibody screening were selectively frozen at −70°C for antibody identification, which was performed on these samples at a later date.
A review of the medical history, obstetric history (including any stillbirths, abortions, medical terminations of pregnancy, and cases of HDFN among siblings), and any past blood transfusions of the alloimmunized patients was conducted. The birth and neonatal follow-up data were recorded. Women who had previous unfavorable fetal outcomes in terms of two or more consecutive spontaneous abortions, fetal deaths, stillbirths, early neonatal deaths, intrauterine growth restriction, and/or congenital anomalies were considered bad obstetric outcomes.
The proposed hypothesis is that alloimmunization in antenatal cases results in bad outcomes and HDFN, and early intervention can help improve outcomes and decrease fetal morbidity and mortality. The outcome measures were to determine the frequency of alloimmunization in pregnant women, the risk of HDFN in the study population, and the prevalence of alloimmunization to red cell antigens in antenatal women attending the ANC clinic. The proportion of minor blood group antibodies was noted, and the benefit of screening for those was analyzed. We propose that timely detection of such antibodies in antenatal women is essential both for the transfusion safety of the mother and for the early management of HDFN.
Data were analyzed using SPSS version 19.0 (SPSS Inc., Chicago, IL, USA). The frequency of red cell alloimmunization in pregnant females, the percentage of specific antibodies, and the risk of HDFN from clinically significant antibodies were calculated. The risk factors for alloimmunization were also noted. Statistical tests were performed using the chi-squared and Fisher’s exact tests.
A total of 2,084 women were screened during this 1.5-year period. The median age of the study population was 25 years (standard deviation: ±4.2) (range, 17-38 years). The distribution of the blood groups in the study population is shown in Table 1. About one-third of women had a B positive blood group phenotype (n=666; 31.95%), and AB negative was the least common blood group phenotype (n=22; 1.05%). Out of all women, 1,765 (84.69%) were Rhesus positive and 319 (15.31%) were Rhesus negative. For 22 mothers, both partners were Rhesus negative.
There were 65 women (3.119%) that alloimmunized to blood group antibodies in the antenatal women attending the ANC in AIIMS Jodhpur. Of those, 54 (2.591%) were sensitized to D antigen, and only 11/2,084 (0.527%) were sensitized to other antigens. The 11 women sensitized to other antigens (16.92% of the total alloimmunized alloantibodies other than anti-D identified in this study) included: anti-M (n=6; 9.23% of all allosensitized), anti-c (n=1; 3.076%), anti-E (n=1; 1.538%), anti-e (n=1; 1.538%), anti-Lewis (a) (n=1; 1.538%), and unspecified antibodies (n =1; 1.538%). Multiple antibodies were seen in four patients that were: combined anti-D and anti-C (n=2; 3.076%), combined anti-e and anti-c (n=1; 1.538%), and combined anti-D and anti-G (n=1; 1.538%). Fig. 1 shows the frequency of alloimmunization and its outcomes. The critical antibody titer in the present study was 1:32.
The mean hemoglobin levels in the study population was 10.952 g/dL. There were 54 (16.92%) alloimmunizations in the D antigen-negative group (n=319), and 11 (0.62%) alloimmunizations in the D antigen-positive group (n=1,765). Thus, a statistically significant difference was found in alloimmunization rates between the D antigen-negative and D-antigen positive groups (16.92% vs. 0.62%, P<0.001). In the study population, 811/2,084 (38.91%) women were primigravida; among those, 13 (0.6238%) tested positive for various antibodies, and 10 (0.479%) were Rh-positive.
Risk factors for alloimmunization were identified in 36/65 females and included the following: 18 out of 65 (27.69%) had a history of abortion, including ectopic pregnancies, and 15 (23.07%) had previous stillbirths/neonatal deaths. Three of 65 alloimmunized females (4.61%) had a history of blood transfusion. The remaining 29 women either did not receive anti-D prophylaxis in a previous pregnancy, or had no identifiable cause for alloimmunization. Four RhD negative women had multiple antibodies.
Forty-two (64.61%) out of 65 females had antibodies that were below the critical titers. Four females in the anti-D group with critical titers also did not have a significant effect on fetuses and newborns. Nineteen women had a clinically significant effect on pregnancy outcome. Thus, the risk of maternal alloimmunization causing HDFN in this study was found to be 19/2,084 (0.9%). The incidence of critical titers of anti-D was 20/319 or 6.2%, and alloimmunization was 16/319 or 5.01% in the D-negative blood types. Of those 16 women, three had combined antibody positivity. One mother was a patient with thalassemia intermedia who had received blood transfusions in the past. The characteristics of mothers having anti-D antibodies are shown in Table 2. There were only 3 mothers in the non-anti-D group who had alloimmunization, which was 0.16% of the Rh-positive mothers and 0.14% of the total study population. The characteristics of the mothers with clinically significant non-anti-D antibodies are shown in Table 3.
In this study, alloantibodies were found in 28/344 (8.1%) of the antenatal women with BOH and in 36/1740 (2.07%) of the antenatal women without any BOH (P<0.01), as shown in Table 4.
In brief outcome and management of pregnancies with alloantibodies the poor outcomes were mainly seen in Ant-D antibody group and remaining antibodies groups did not required intensive care (Table 5). Thus D alloantibodies should be monitored carefully if diagnosed in any antenatal women.
Rh isoimmunization is a solvable problem whose burden has been reduced in countries with a high socioeconomic status, but remains a problem in middle and low socioeconomic countries [10,11]. India needs to formulate guidelines that can help reduce the HDFN burden, while at the same time being cost-effective. Currently, detailed identification facilities for antibodies other than anti-D are not available in most centers. However, large-scale studies on pregnant women should be conducted to collect sufficient evidence to formulate guidelines and define indications for alloantibody screening and identification.
Alloimmunization is influenced by age at prior transfusion, the number of blood transfusions, major surgery, multiparity, prior male child, and prior operative removal of placentae [12-15]. Thus careful transfusions to women of reproductive age is an important step for reducing the incidence of alloimmunization. The factors in a current pregnancy that may increase the probability of alloimmunization are an insufficient dose of Rh-immunoglobulin, feto-maternal hemorrhage such as caesarean section, assisted vaginal delivery, and post-maturity [13,16]. The prevalence of red cell antibodies in any population also alters the rate of alloimmunization. For instance, the prevalence of the RhD blood group in any population may vary, from as high as 15-17% in the European/North American population to 3-8% in the African and Indian races, and can be very low (0.1-0.3%) in Asian countries [12]. This rate is highly variable from 4.8% to 21.8% in the Indian population, as noted in various studies. The observed prevalence of the RhD blood group in the current study population was 15.31%. A similarly high prevalence was noted in tertiary care centers by Das et al. [10], Basu et al. [4], and Al-Ibrahim and Al Saeed [17]. The details of alloimmunization from various studies are presented in Table 6.
The alloimmunization rate during pregnancy observed in the current study was 3.119%. This is higher than other Indian studies that have reported a rate between 1.1-2.27%. This can be explained by the fact that the present study was conducted in a tertiary care center with fetal medicine facilities. Thus, as the study population included more referred cases, there were more high-risk pregnancies than in the general population. This is the reason for the higher alloimmunization rate in both Rh-negative and Rh-positive subgroups. RhD antigen sensitization was responsible for 83.08% of total alloimmunizations. The alloimmunization rate was 16.92% in the Rh-negative subgroup, and 0.62% in the Rh-positive subgroup. Thus, even decades after the advent of RhD prophylaxis, RhD antibodies remain the most common causal factor of alloimmunization and one of the antigens that cause severe HDFN [18]. Most of the Indian population, especially the rural population, is still unaware of the effect of the Rh-negative blood group on the pregnancy and fetus. The anti-D immunoprophylaxis rate in India after any sensitizing event like an abortion is very low (10-20%) [4]. This data emphasize that along with anemia, hypertension, and diabetes in pregnancy, the government of India should propagate awareness about alloimmunization, which is an avoidable cause.
Antibodies other than anti-D in this study included anti-M, anti-E, anti-e, and anti-c. Anti-M was the most common non-anti-D antibody in 6 mothers. Of the six anti-M antibodies, 5 mothers had normal pregnancy outcomes, while one had critical titers and developed pathological jaundice. This patient also had BOH, thus exhibiting severe alloimmunization. Anti-M is a naturally occurring immunoglobulin M antibody that reacts in cold and is clinically insignificant [1,19]. Its conversion to IgG is rare and can cause HDFN. The prevalence of anti-M can be 10-15% in the pregnant population, but the incidence of HDFN associated with anti-M is very low [1,2]. Rai et al. [1] reported a case of severe alloimmunization with anti-M antibody.
Anti-E is reported to be one of the common Rh non-anti-D antibodies causing mild to moderate HDFN [3,20]. In addition, there are reports of anti-e causing HDFN [21]. In this study, anti-E caused mild HDFN, even in high titers.
Anti-C antibody is rarely seen alone, and is usually found in association with anti-D and anti-E [3]. The present study also found two cases of combined anti-C and anti-D, both of which had severe HDFN. Thus, in this study, 11 patients had non-D antibodies, and only three (0.14% of the study population) had features of HDFN. This shows that non-anti-D alloimmunization is very low compared to anti-D alloimmunization, and these antibodies were less severe compared to D antibodies.
In India, alloimmunization remains an important cause of HDFN. Most studies from India and worldwide have found that the alloimmunization rate was significantly higher in the BOH group compared to the normal group [3,4,6,17,22]. The same was true in this study: 8.1% of females with BOH had alloimmunization, compared to 2.07% of women without BOH. Thus, screening for antibodies in women with BOH is necessary, rather than performing universal antenatal screening.
As non-anti-D antibodies have a lower incidence and are less severe than anti-D antibodies, and looking at the cost-benefit ratio, it is justified to perform antibody screening only in Rh-negative mothers and those with BOH, as most alloimmunizations were found in these groups. There is an urgent need to initiate programs and campaigns to increase awareness of alloimmunization and anti-D prophylaxis among the common population of India. To this end, Rh-negative pregnancies should be included in mother-child programs run by the Indian government.
Sánchez-Durán et al. [23] in their study classified alloimmunized pregnancies as low- and high-risk by stratifying for the severity of fetal anemia and the need for intrauterine transfusion. Treatments like intrauterine transfusion, phototherapy, and intravenous immunoglobulin have helped reduce the severity of HDFN [4]. The determining factors included the type and titer of the antibody, paternal phenotype, and fetal antigen. This helps in considering low-risk groups for routine follow-up, thus reducing stress and disease burden, while on the other hand the stringent follow-up of high-risk cases with middle cerebral artery (MCA) peak systolic velocity (PSV) will allow timely intervention to the needy high-risk fetus. In their study, the critical titers were 1:16 as opposed to 1:32 in the present study.
Also, 36.9% of the total alloimmunized cases had critical titers and were at high risk, and features of HDFN were seen in those cases in the current study. Thus, the remaining 63.1% can be categorized as low risk. Interventions such as serial ultrasound follow-up of the MCA PSV, intrauterine transfusions, neonatal exchange transfusions, and phototherapy were administered to these high-risk fetuses.
The current study included only hospital patients and does not represent the prevalence of anti-D among the large number of Indian women who do not have access to obstetric care. Any additional population-specific antigens that might explain the substantial proportion of unidentified antibodies in the current research must be investigated further. However, there is still a remote possibility that more antibodies go unreported/unidentified owing to restrictions in facility identification. The incidence reported in this study can be slightly higher than that of the normal pregnant population in this area, as the study was conducted at a tertiary care referral center mostly dealing with high-risk pregnancies.
In developing countries such as India, universal antenatal antibody screening, though desirable, may not be justified at present, as the cost and infrastructure required would be immense. However, it is necessary to impose properly formulated protocols to at least screen pregnant women with BOH. Antenatal anemia is another risk factor for receiving blood transfusion that causes alloimmunization during pregnancy; therefore, antenatal anemia correction is an easily modifiable factor for reducing alloimmunization in pregnancy. Classifying pregnancies as low- or high-risk for fetal anemia can help in the pregnancy follow-up, and can result in better feto-maternal outcome. Pregnancies with high antibody titers may require intensive perinatal and neonatal treatments.
Notes
Fig. 1
Flowchart showing distribution of alloantibodies in the study population and its outcomes. IUT, intrauterine transfusion.
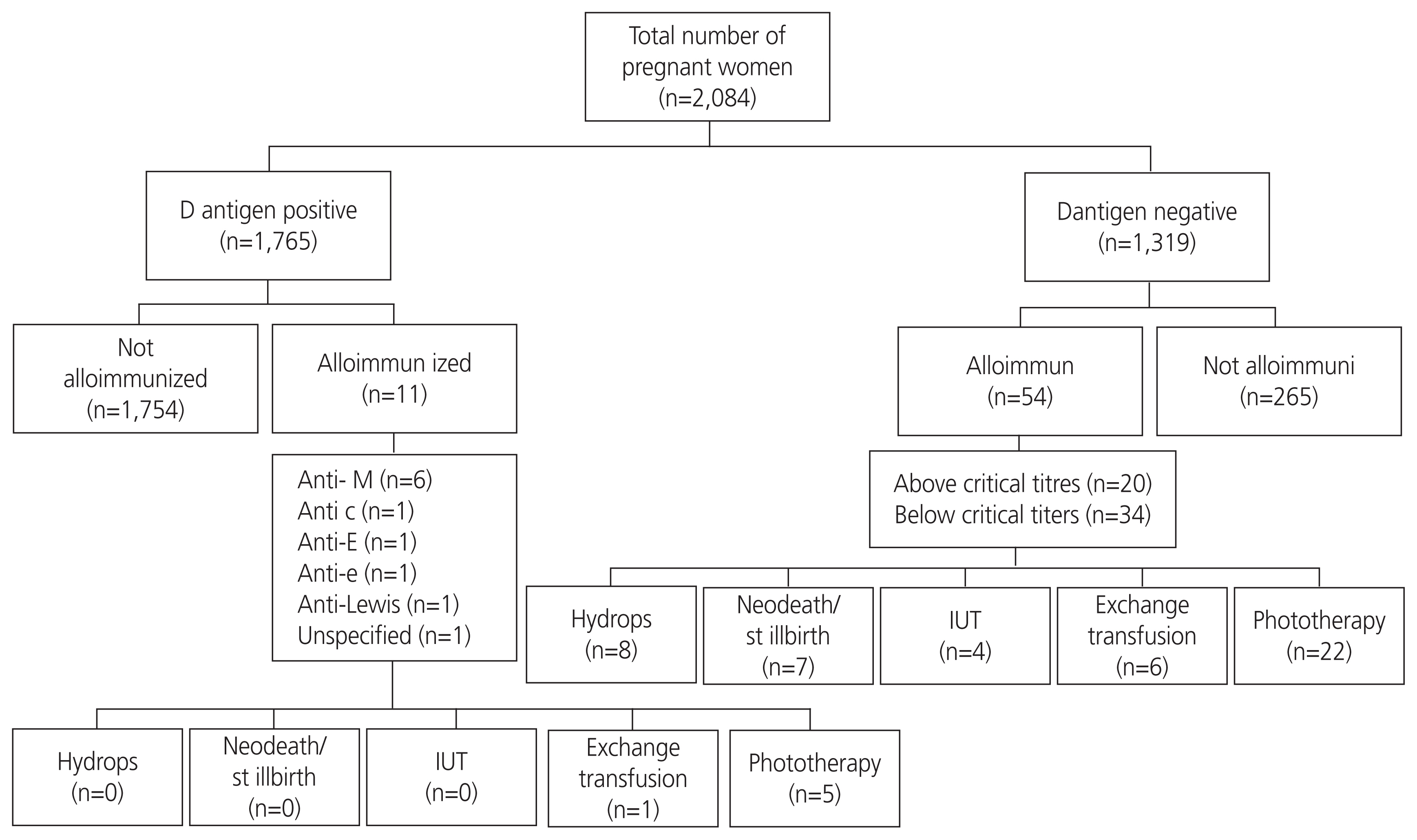
Table 1
Frequency of blood groups in the study population (n=2,084)
Table 2
Clinical profile of mothers having anti-D antibody
Table 3
Characteristics of mothers having clinically significant non-anti-D antibodies identified
Table 4
Distribution of alloantibodies in pregnant women
| Presence of alloantibodies | Total antenatal women | Statistical valuea) | |
|---|---|---|---|
| D-antigen negative | 54 (16.92) | 319 | P<0.001 |
| D-antigen positive | 11 (0.62) | 1,765 | P<0.001 |
| With bad obstetric history (BOH) | 28 (8.10) | 344 | P<0.01 |
| Without BOH | 36 (2.07) | 1,740 | P<0.001 |
Table 5
Distribution of alloantibodies in pregnant women and their effects on clinical management
Table 6
Comparison of alloimmunization rate from reported studies
| Study | Country | Year of study | Sample size | Prevalence of Rh negative | Alloimmunization rate in the study population | Alloimmunization rate in Rh negative | Alloimmunization rate in Rh positive | Alloimmunization rate in BOH |
|---|---|---|---|---|---|---|---|---|
| Dholakiya et al. [22] | Gujrat, India | 2014 to 2016 | 8,920 | 4.8 | 1.3 | 19.4 | 0.3 | 5 |
| Suresh et al. [3] | Tirupati, India | 2012 to 2013 | 2,060 | 6.5 | 1.1 | 12.8 | 0.3 | 1.9 |
| Basu et al. [4] | Karnataka, India | 2013 to 2015 | 2,336 | 21.8 | 2.3 | 6.9 | 1.1 | 0.9 |
| Varghese et al. [9] | Vellore, India | 2008 to 2009 | 5,347 | 6.3 | 1.5 | 9.4 | 0.1 | |
| Pahuja et al. [6] | New Delhi, India | 2008 to 2009 | 3,577 | 11.0 | 1.3 | 10.7 | 0.1 | 5.5 |
| Altuntas et al. [24] | Turkey | 2006 to 2012 | 4,840 | 15.3 | 8.7 | |||
| Al-ibrahim and Al Saeed [17] | Saudi Arabia | 2008 | 1,195 | 2.0 | ||||
| Gottvall and Filbey [25] | Sweden | 1992 to 2005 | 78,125 | 0.5 | ||||
| Karim et al. [2] | Pakistan | 2014 | 1,000 | 13.6 | 1.8 | 2.9 | 1.6 | |
| Koelewijn et al. [26] | Netherland | 2002 to 2004 | 305,000 | 1.2 | 0.4 | |||
| Present study | Rajasthan India | 2019 to 2021 | 2,084 | 15.3 | 3.2 | 17.2 | 0.6 | 8.1 |
References
1. Rai R, Saha SC, Jain A, Bagga R, Kumar P, Marwaha N. Anti-M alloimmunization in pregnancy: an unusual cause of bad obstetric history. J Obstet Gynaecol India 2016;66:607-9.




2. Karim F, Moiz B, Kamran N. Risk of maternal alloimmunization in Southern Pakistan - a study in a cohort of 1000 pregnant women. Transfus Apher Sci 2015;52:99-102.


3. Suresh B, Babu KVS, Arun R, Jothibai DS, Bharathi T. Prevalence of “unexpected antibodies” in the antenatal women attending the Government maternity hospital, Tirupati. J Clin Sci Res 2015;4:22-30.

4. Basu S, Kaur R, Kaur G. Hemolytic disease of the fetus and newborn: current trends and perspectives. Asian J Transfus Sci 2011;5:3-7.



5. Zipursky A, Paul VK. The global burden of Rh disease. Arch Dis Child Fetal Neonatal Ed 2011;96:F84-5.


6. Pahuja S, Gupta SK, Pujani M, Jain M. The prevalence of irregular erythrocyte antibodies among antenatal women in Delhi. Blood Transfus 2011;9:388.


7. ACOG Practice Bulletin No. 192: management of alloimmunization during pregnancy. Obstet Gynecol 2018;131:e82-90.


8. White J, Qureshi H, Massey E, Needs M, Byrne G, Daniels G, et al. Guideline for blood grouping and red cell antibody testing in pregnancy. Transfus Med 2016;26:246-63.


9. Varghese J, Chacko MP, Rajaiah M, Daniel D. Red cell alloimmunization among antenatal women attending a tertiary care hospital in south India. Indian J Med Res 2013;138:68-71.


10. Das S, Shastry S, Rai L, Baliga PB. Frequency and clinical significance of red cell antibodies in pregnancy - a prospective study from India. Indian J Pathol Microbiol 2020;63:241-6.


12. Webb J, Delaney M. Red blood cell alloimmunization in the pregnant patient. Transfus Med rev 2018;32:213-9.


13. Koelewijn JM, Vrijkotte TG, de Haas M, van der Schoot CE, Bonsel GJ. Risk factors for the presence of nonrhesus D red blood cell antibodies in pregnancy. BJOG 2009;116:655-64.


14. Schonewille H, Van De Watering LM, Loomans DS, Brand A. Red blood cell alloantibodies after transfusion: factors influencing incidence and specificity. Transfusion 2006;46:250-6.


15. Verduin EP, Brand A, Middelburg RA, Schonewille H. Female sex of older patients is an independent risk factor for red blood cell alloimmunization after transfusion. Transfusion 2015;55:1478-85.


16. Koelewijn JM, de Haas M, Vrijkotte TG, van der Schoot CE, Bonsel GJ. Risk factors for RhD immunisation despite antenatal and postnatal anti-D prophylaxis. BJOG 2009;116:1307-14.



17. Al-Ibrahim NA, Al Saeed AH. Red blood cell alloimmunization among Saudi pregnant women in the central province of Saudi Arabia. Kuwait Med J 2008;40:116-23.
18. de Haas M, Thurik FF, Koelewijn JM, van der Schoot CE. Haemolytic disease of the fetus and newborn. Vox Sang 2015;109:99-113.


19. Devi SA, Alwar VA, Sitalakshmi S, Rameshkumar K, Mhaskar R. Red blood cell antibody screening in pregnancy. Asian J Transfus Sci 2011;5:56.



20. Jeremiah ZA, Mordi A, Buseri FI, Adias TC. Frequencies of maternal red blood cell alloantibodies in Port Harcourt, Nigeria. Asian J Transfus Sci 2011;5:39-41.



21. Kumawat V, Jain A, Sharma RR, Marwaha N. Hemolytic disease of fetus and newborn due to anti-E alloantibody in a newborn of Rh (D)-positive mother. Asian J Transfus Sci 2012;6:187.



22. Dholakiya SK, Bharadva S, Vachhani JH, Upadhyay BS. Red cell alloimmunization among antenatal women attending tertiary care center in Jamnagar, Gujarat, India. Asian J Transfus Sci 2021;15:52-6.



23. Sánchez-Durán MÁ, Higueras MT, Halajdian-Madrid C, Avilés García M, Bernabeu-García A, Maiz N, et al. Management and outcome of pregnancies in women with red cell isoimmunization: a 15-year observational study from a tertiary care university hospital. BMC Pregnancy Childbirth 2019;19:1-8.




24. Altuntas N, Yenicesu I, Himmetoglu O, Kulali F, Kazanci E, Unal S, et al. The risk assessment study for hemolytic disease of the fetus and newborn in a University Hospital in Turkey. Transfus Apher Sci 2013;48:377-80.























