|
 |
- Search
| Obstet Gynecol Sci > Volume 58(6); 2015 > Article |
Abstract
Objective
To evaluate the safety and surgical outcomes of laparoscopically assisted vaginal hysterectomy (LAVH) for women with anterior wall adherence after cesarean section.
Methods
We conducted a retrospective study of 328 women with prior cesarean section history who underwent LAVH from March 2003 to July 2013. The subjects were classified into two groups: group A, with anterior wall adherence (n=49); group B, without anterior wall adherence (n=279). We compared the demographic, clinical characteristics, and surgical outcomes of two groups.
Results
The median age and parity of the patients were 46 years (range, 34 to 70 years) and 2 (1 to 6). Patients with anterior wall adherence had longer operating times (175 vs. 130 minutes, P<0.05). There were no significant differences in age, parity, number of cesarean section, body mass index, specimen weight, postoperative change in hemoglobin concentration, or length of hospital stay between the two groups. There was one case from each group who sustained bladder laceration during the vaginal portion of the procedure, both repaired vaginally. There was no conversion to abdominal hysterectomy in either group.
Cesarean section is the most commonly performed abdominal surgery on women in the US and Korea. In 2011, one-third of all deliveries were performed by cesarean section in Korea and the US [1,2]. As the rate of cesarean section has increased, more women with a history of cesarean section undergo subsequent surgery. Such women may have various adhesions between any of the organs including small intestine, colon, rectum, pelvic peritoneum, omentum, adnexae, and uterus, which often complicate the process during abdominal or pelvic surgery [3].
Hysterectomy is a commonly performed surgery in gynecologic field. It requires the mobilization of the urinary bladder off the cervix to minimize the risk of a potential vesicovaginal fistula and to reduce urinary bladder injury. Hysterotomy scars from the cesarean section can result in adhesions between the urinary bladder and anterior abdominal wall, making bladder mobilization much more difficult. Accordingly, there have been reports that there is a higher probability of bladder injury and conversion to laparotomy during hysterectomy among women who have a history of cesarean section than among those who do not. Hence, such women with history of cesarean sections are sometimes recommended laparotomic surgery in the first place [4,5,6].
This study aimed to evaluate the safety and surgical outcomes of laparoscopically assisted vaginal hysterectomy (LAVH) for women with anterior wall adherence after cesarean section.
We conducted a retrospective chart review of 328 women with prior cesarean section history who underwent LAVH for benign gynecologic diseases from March 2003 to July 2013 in two university teaching hospitals, selected from a total of 2,034 women who underwent LAVH during that period. All LAVHs were performed by two experienced gynecologic surgeons. The subjects were classified into two groups: group A, with anterior wall adherence (n=49); group B, without anterior wall adherence (n=279).
We analyzed data on patients' age, parity, body mass index, indications for hysterectomy, number of prior cesarean sections, histopathological results, the change in hemoglobin concentration from before surgery to postoperative day 1, conversion to laparotomy, weight of the resected uterus, operating time, hospital stay, and any complications.
The inclusion criteria for performing LAVH were as follows: (1) Patients with 'menorrhagia' who were diagnosed with symptomatic uterine myoma or adenomyosis. Other possible causes of menorrhagia, such as cervical or endometrial cancer, were examined and excluded. (2) Patients who presented to the hospital with 'chronic pelvic pain' in association with uterine myoma or adenomyosis. (3) Patients who initially visited the hospital complaining of 'palpable abdominal mass' and were later diagnosed with grown uterine myomas. (4) Patients who were diagnosed with benign uterine disease other than uterine myoma. (5) Patients who were diagnosed with benign ovarian tumors.
We perform LAVH and both salpingooophorectomy in benign ovarian tumor cases with following indications: patients older than 60 years of age, cases with underlying uterine myomas or adenomyosis, uterine prolapse, and cases with uncertain frozen section analysis with suspected malignancy or borderline malignancy.
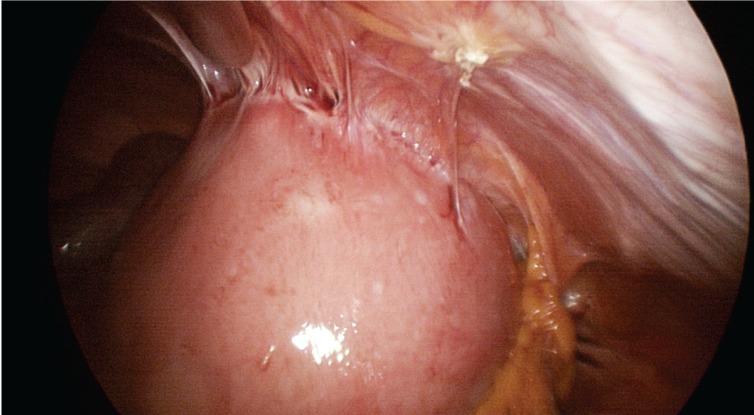
The operating time was defined as the time from the insertion of the first trocar to closure of all port sites. The diagnosis of anterior wall adherence was based on laparoscopic surgical images (Fig. 1). The Kangbuk Samsung Hospital and the Hanyang University Hospital Institutional Review Boards both approved this study.
A preoperative bowel preparation with Fleet Phospho-soda (CB Fleet Co. Inc., Lynchburg, VA, USA) was performed in all cases. To make a pneumoperitoneum safely, a lateral approach was used in which a Veress needle or a 5-mm trocar was inserted directly into the left upper quadrant, lateral to the inferior and superior epigastric vessels between the umbilicus and the epigastric area. After creating a pneumoperitoneum, a 5-mm telescope was used to examine the intra-abdominal cavity to locate any adhesions, especially anterior wall adherence. A second trocar was inserted in the right upper quadrant for women with anterior wall adherence. An infraumbilical trocar (no.1 trocar) was inserted when there was no severe adhesion beneath the patient's umbilicus. If there was an umbilical adhesion, the telescope was moved to the right upper quadrant port site (no. 3 trocar) to secure a good visual field; a dissecting Metzenbaum scissors with monopolar coagulation was used via the left upper quadrant port (no. 2 trocar) for adhesiolysis, and then the infraumbilical trocar was inserted. We started adhesiolysis and hysterectomy after inserting the three trocars.
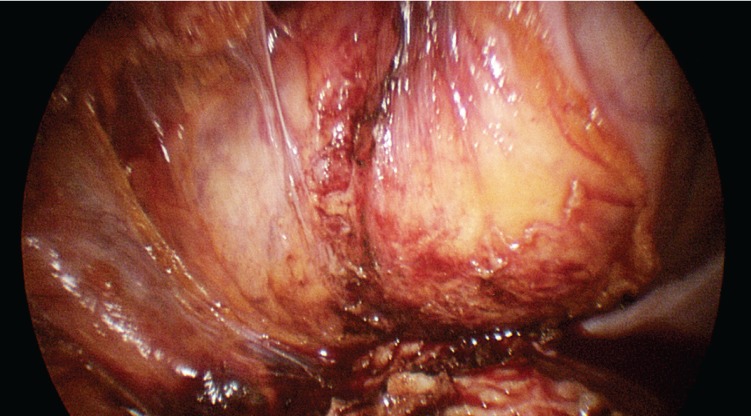
The ovarian ligaments, round ligaments, and broad ligament were cut and dissected after ligating using laparoscopic extracorporeal knot-tying techniques [7]. The laparoscopic procedures included dissecting the broad ligament in front of the uterine artery, opening the bladder flap, and dissecting the bladder peritoneum. If the space between the urinary bladder and the uterine lower segment was unclear while moving towards the uterine cervix, a Foley catheter was used to introduce approximately 150 to 200 mL of normal saline or carbon dioxide (Fig. 2). The remaining vaginal procedures were performed as described for LAVH in our previous report [8]. After hysterectomy, the abdominal cavity was insufflated again with carbon dioxide and laparoscopically washed with normal saline solution. After confirming the ureteral peristalsis and bleeding, a Jackson-Pratt drain drainage tube was inserted through the 5-mm trocar, and the gas was removed.
Data are expressed as medians (ranges). The data were analyzed using SPSS ver. 17.0 (SPSS Inc., Chicago, IL, USA). Frequency distributions were compared using chi-squared test, and median values were compared using the Mann-Whitney nonparametric U-test. P<0.05 (two-sided) was considered significant.
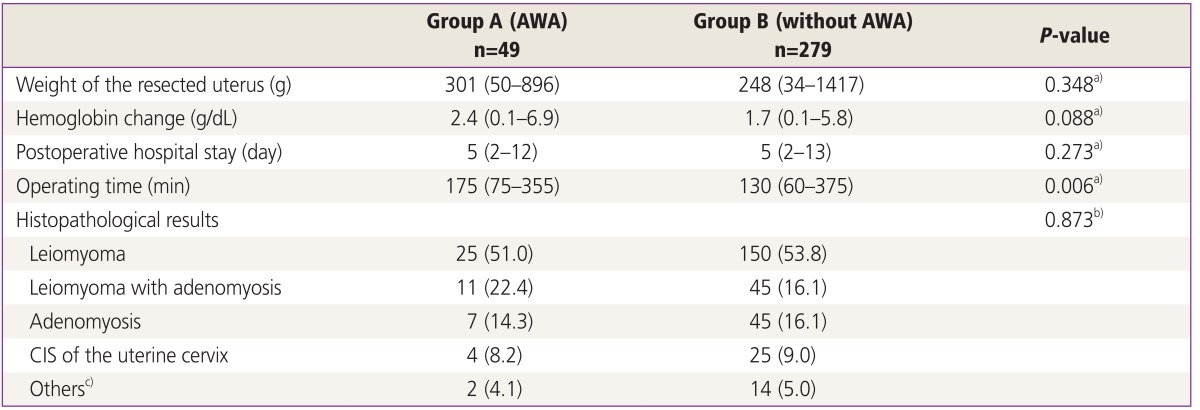
Of the total 328 patient, forty-nine (14.9 %) patients had anterior wall adherence. The median age and parity of the patients were 46 years (range, 34 to 70 years) and 2 (1 to 6). The median number of cesarean sections was 1 (range, 1 to 3). The indications for LAVH (ordered by frequency) were menorrhagia, chronic pelvic pain, palpable abdominal mass, and squamous cell carcinoma in situ of the uterine cervix. The demographic characteristics did not differ between the two groups (Table 1).
The specimen weight, postoperative change in hemoglobin concentration, and length of hospital stay did not differ between the two groups. Patients with anterior wall adherence required longer operating times than those without (175 vs. 130 minutes, P<0.05) (Table 2).
There was one case from each group who sustained bladder laceration during the vaginal portion of the procedure, both repaired vaginally. There was no conversion to abdominal hysterectomy in either group.
Adhesions have been observed among 46% to 65% of women having a repeat cesarean section after a primary cesarean section [9]. Abdominal and pelvic adhesions can be asymptomatic in most cases. However, some patients could have symptoms ranging from chronic pelvic pain, dyspareunia, infertility to small bowel obstruction that sometimes requires adhesiolysis [10]. More severe adhesions occur with increasing numbers of cesarean section. In such cases, additional adhesiolysis might be required during surgery and this could extend the operative time along with the increased possibility of more blood loss and prolonged hospital stay [11,12].
Dense adhesions between the anterior abdominal wall and uterus-anterior wall adherence-have been continually reported since the first report by Sheth et al. [13]; about eight cases found upon subsequent surgery on women with a history of prior cesarean section. Anterior wall adherence makes free movement during bimanual pelvic examination difficult due to adhesion of the uterus to the anterior wall. The uterine cervix is found at a location closer to the superior side. Furthermore, speculum examination reveals that the vaginal wall is pulled upward; hence, the uterine cervix is invisible because of its high position, which makes it difficult to observe even with the use of other instruments. Traction of the uterine cervix with a tenaculum may also reveal dimpling of the lower abdominal skin or a cesarean section scar. Such pelvic and physical examination findings in patients with prior cesarean section were named the cervicofundal sign.
Anterior wall adherence can be diagnosed through imaging studies, such as ultrasonography or magnetic resonance imaging performed before surgery. Women with a history of prior cesarean section might be suspected to have anterior wall adherence when there is a wide horn-shaped uterus peaking from the uterine fundus to the anterior abdominal wall (uterine peaking sign) or if the uterus appears to protrude into the abdominal wall through a gap between the uterus and rectus abdominis muscles when observed using pelvic sonography [13,14,15]. It can also be diagnosed when the anterior wall of the uterus adheres to the anterior abdominal wall with evidence of obliteration of the fat plane, or when the uterine cervix is elongated facing the upper third of the posterior vaginal wall and located posterior to the bladder on magnetic resonance imaging (Fig. 3).
Most cases of anterior wall adherence are found during gynecologic surgery or repeated cesarean sections. In such case, adhesiolysis must be performed to approach the pelvic cavity and to perform an appropriate surgery. During laparoscopic surgery, sufficient adhesiolysis must be performed first to secure the visual field and produce space to safely insert the umbilical trocar and other trocars for the surgery. Additionally, most women who undergo hysterectomy for symptomatic uterine fibroids that further limits the space within the pelvic cavity and prolongs the time taken for adhesiolysis. Women with anterior wall adherence often have the uterine cervix pulled upward, as mentioned before; in such cases it will be difficult to insert a uterine manipulator. As a result, traction of the uterus, which is important during hysterectomy becomes difficult. Likewise, securing the visual field and space become challenging during laparoscopic surgery, ultimately extending the time required for adhesiolysis.
Based on these surgical results, the following techniques are suggested for safe LAVH surgery in women with anterior wall adherence caused by prior cesarean section. The first consideration is placement of the initial trocar superiorly or cephalad on the abdominal wall. A patient expected to have anterior wall adherences is also likely to have adhesion to the umbilical level. Even if there is no adhesion to the umbilicus, the distance from the telescope inserted through the umbilical trocar to the adhered uterus is sometimes too close to secure a sufficient visual field for adhesiolysis. In such cases, insertion of the first trocar at the upper lateral part Palmer's point will enable the surgeon to make a pneumoperitoneum safely [16]. If there are adhesions around the umbilicus, the trocar can be inserted by avoiding such area. Using two upper lateral ports (no. 2 and 3 trocars) and an umbilical trocar (no. 1 trocar) allows the surgeon to use both hands during the surgery by staying on the left side of the patient, as stated in our port placement method.
The second point is the injection of 150 to 200 mL of normal saline infusion or carbon dioxide through a Foley catheter to distend the bladder when the boundary between the urinary bladder and the adhesion site is unclear [17]. The margin of the urinary bladder can be visualized either by injecting saline via a syringe connected to the catheter or injecting carbon dioxide gas by attaching a laparoscopic gas insufflation tube directly to the catheter after clamping the Foley catheter. In our experience, when the urinary bladder margin had to be checked during dissection, injection of normal saline was satisfactory but carbon dioxide insufflation tube was more convenient and less time consuming. Injection of the gas sufficiently distended the urinary bladder thus clearing the muscularis around the bladder, which enabled the examination of the plane for dissection in addition to frequent insufflation and desufflation. This method use in this series of patients decreased the risk of bladder injury and enabled safe mobilization of the bladder. Following dissection, carbon dioxide or normal saline insufflation was used again to check the urinary bladder margin, and, as expected, the carbon dioxide insufflation method proved to be convenient.
In conclusion, our experience confirms that LAVH for women with prior cesarean section may take 45 minutes longer in the presence of anterior wall adhesions, but it is a safe and efficient approach for hysterectomy, if performed with careful dissection techniques.
References
1. Hamilton BE, Martin JA, Ventura SJ. Births: preliminary data for 2012. Natl Vital Stat Rep 2013;62:1-20.
2. Health Insurance Review and Assessment Service. 2011 National Health Insurance statistical yearbook. Seoul: Health Insurance Review and Assessment Service; 2012.
3. Sinha R, Sundaram M, Lakhotia S, Hedge A, Kadam P. Total laparoscopic hysterectomy in women with previous cesarean sections. J Minim Invasive Gynecol 2010;17:513-517. PMID: 20621012.


4. Chang WC, Hsu WC, Sheu BC, Huang SC, Torng PL, Chang DY. Minimizing bladder injury in laparoscopically assisted vaginal hysterectomy among women with previous cesarean sections. Surg Endosc 2008;22:171-176. PMID: 17522923.


5. Walid MS, Heaton RL. Total laparoscopic hysterectomy with obliterated anterior cul-de-sac. Ger Med Sci 2010;8:Doc03PMID: 20200656.


6. Rooney CM, Crawford AT, Vassallo BJ, Kleeman SD, Karram MM. Is previous cesarean section a risk for incidental cystotomy at the time of hysterectomy? A casecontrolled study. Am J Obstet Gynecol 2005;193:2041-2044. PMID: 16325612.


7. Pasic R, Levine RL. Laparoscopic suturing and ligation techniques. J Am Assoc Gynecol Laparosc 1995;3:67-79. PMID: 9050619.


8. Choi JS, Kyung YS, Kim KH, Lee KW, Han JS. The fourtrocar method for performing laparoscopically-assisted vaginal hysterectomy on large uteri. J Minim Invasive Gynecol 2006;13:276-280. PMID: 16825066.


9. Lyell DJ. Adhesions and perioperative complications of repeat cesarean delivery. Am J Obstet Gynecol 2011;205(6 Suppl):S11-S18. PMID: 22114993.


10. Szomstein S, Lo Menzo E, Simpfendorfer C, Zundel N, Rosenthal RJ. Laparoscopic lysis of adhesions. World J Surg 2006;30:535-540. PMID: 16555020.


11. El-Shawarby SA, Salim R, Lavery S, Saridogan E. Uterine adherence to anterior abdominal wall after caesarean section. BJOG 2011;118:1133-1135. PMID: 21481158.


12. Hirschelmann A, Tchartchian G, Wallwiener M, Hackethal A, De Wilde RL. A review of the problematic adhesion prophylaxis in gynaecological surgery. Arch Gynecol Obstet 2012;285:1089-1097. PMID: 22037682.


13. Sheth SS, Goyal MV, Shah N. Uterocervical displacement following adhesions after caesarean section. J Gynecol Surg 2009;13:143-147.
14. Sheth SS, Shah NM, Varaiya D. A sonographic and clinical sign to detect specific adhesions following caesarean section. J Gynecol Surg 2008;24:27-36.

15. Walid MS, Heaton RL. Uterine peaking: sonographic sign of vesico-uterine adhesion. Ger Med Sci 2011;9:Doc24PMID: 21921998.


16. Chang FH, Lee CL, Soong YK. Use of palmer's point for insertion of the operative laparoscope in patients with severe pelvic adhesions: experience of seventeen cases. J Am Assoc Gynecol Laparosc 1994;1(4, Part 2):S7PMID: 9073666.

17. O'Hanlan KA. Cystosufflation to prevent bladder injury. J Minim Invasive Gynecol 2009;16:195-197. PMID: 19138575.


-
METRICS

-
- 2 Crossref
- 2,782 View
- 29 Download
- Related articles in Obstet Gynecol Sci
-
Laparoscopically Assisted Vaginal Hysterectomy: A Review of 43 Cases.1998 October;41(10)