|
 |
- Search
| Obstet Gynecol Sci > Volume 58(1); 2015 > Article |
Abstract
Objective
The purpose of this study was to investigate the aortic isthmus (AoI) flow difference between larger fetus and smaller fetus of twin; and to evaluate the predictive value of early diagnosis of hemodynamic change in twin growth.
Methods
This prospective study on 49 pairs of twin fetuses was performed to obtain AoI blood flow data. Cases with structural or chromosomal abnormalities and co-twin death were excluded. The interval from examination to delivery was within 4 weeks and 3 cases over 4 weeks interval were re-examined. Assessment of fetal AoI Doppler parameters were peak systolic velocity (PSV), end-diastolic velocity, times-averaged maximum velocities, pulsatility index (PI), and resistance index (RI). According to the direction of the diastolic flow in the AoI, antegrade and retrograde flow were made and was used to analyze the perinatal outcomes of each fetus. The predictive value of AoI Doppler parameters in predicting fetal growth was obtained by using ANOVA and logistic regression analysis of quantitative variables in each fetus of twins.
Results
There were significant differences in the gestational weeks at delivery, birth weight and the incidence of growth discordance over 20% or more between monochorionic twin and dichorionic twin. The AoI PI and RI were significantly higher in smaller fetus than in larger regardless of chorionicity. Retrograde flow was noted in 8 of 98 cases (8.2%) and the only one case was of the larger fetus and the others were smaller fetuses of twin. Significant correlations were found between the AoI PI and birthweight (P=0.018) and between the PSV and growth discordance (P=0.032). In monochorionic twin, linear correlation was shown between the AoI PI and birthweight (P=0.004) and between AoI PI and growth discordance (P=0.031). Also, the meaningful correlation between the PSV and birthweight (P=0.036) was found by using logistic regression analyses.
The aortic isthmus (AoI) is the vascular segment located between the origin of the left subclavian artery and the aortic end of the ductus arteriosus. The AoI has been suggested to be the only arterial connection between the right and left fetal vascular systems [1]. In placental insufficiency, the fetal circulation shows preferential redistribution of the arterial circulation of cardiac output toward the left ventricle, which maintains an adequate oxygen supply to both brain and the heart. Doppler examination of the umbilical artery and the middle cerebral artery (MCA) have proved to be good predictors of adverse perinatal outcomes. Venous Doppler patterns such as revered flow in the ductus venousus (DV) and atrial pulsations in the umbilical vein have been advocated as the best predictors of adverse perinatal outcome [2,3]. The AoI flow as an indicator of the progression of fetal hemodynamic deterioration in fetuses has been proposed [4].
Discordant twin growth made on serial ultrasound examinations can predict adverse pregnancy outcome. Especially in a smaller fetus of discordant twin, there is a much higher risk for adverse outcome than in an appropriate size of twin fetus [5,6]. Such this discordance usually results from unequal placentation, umbilical cord abnormalities and fetal malformation in dizygotic twins, and vascular anastomses within the placenta in monozygotic twins [7]. Currently there are no reports on the study of AoI flow in the twin with discordant growth, where the discordant growth is caused by the hemodynamic imbalance.
The purpose of our study is to investigate the AoI blood flow difference between the larger fetus and smaller fetus in twin and the additionally showed the difference of AoI flow by chorionicity and finally to evaluate the clinical usefulness of hemodynamic change in twins.
This prospective study on twin fetuses was performed between November 2008 and December 2009. The AoI data was obtained from 49 twin pairs (74.4%) out of 66 twins delivered at our hospital during this period. The remaining 17 twins were excluded due to several reasons. In some cases, the AoI images were inappropriate as it was available only to one twin fetus due to fetal position. In other cases, it was unable to measure the AoI blood flow due to the immediate deliveries transferred from another hospital.
The research protocol was approved by the local ethics committee and all subjects gave their informed consent to participate. Gestational age was confirmed by sonographic examination in the first trimester in all cases. There were no cases with structural or chromosomal abnormalities and co-twin death. And there were no twin-to-twin transfusion syndrome in our twins. The mean gestational age to perform Doppler examination was 29.4 weeks (range between 21 and 36 weeks of gestation). The interval from examination to delivery was within 4 weeks. Three cases of over 4 week's interval were re-examined AoI blood flow values and a last result was used for analysis. Image-directed pulsed and color Doppler equipment (ATL HDI 5000 Philips, USA) with a multifrequency sector array transabdominal transducer was used.
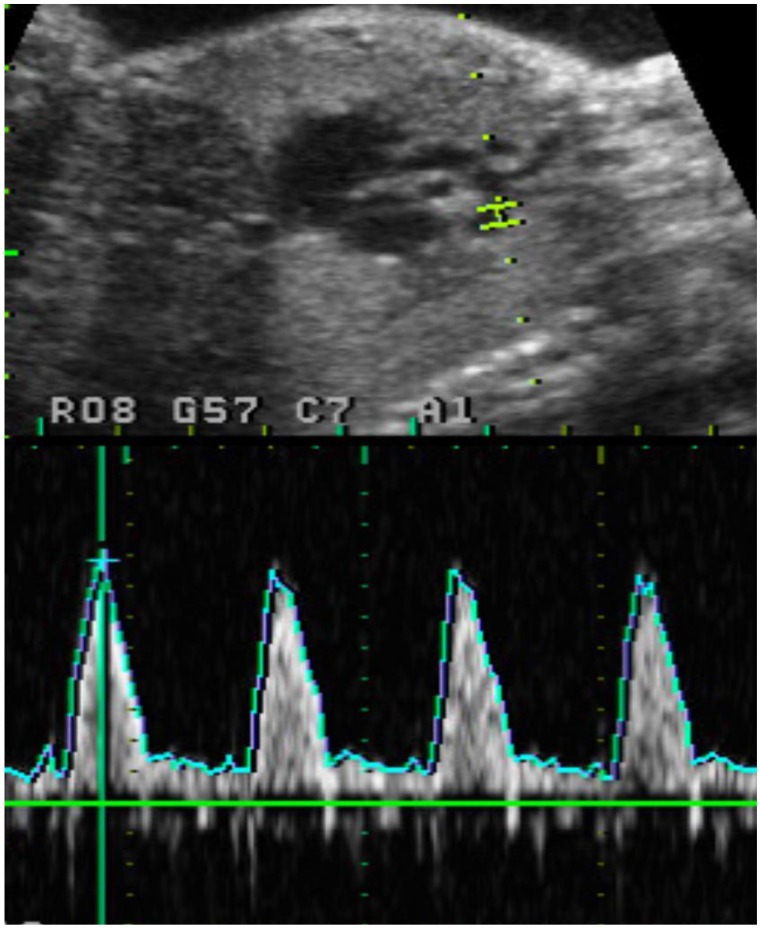
The technique of Doppler blood flow of the fetal AoI was as follows: from a horizontal 4-chamber view of the fetal heart, a 90-degree rotation of the transducer provides a saggital view of the fetus on which the aortic arch can be observed. The isthmus is then identified between the origin of the left subclavian artery and the aortic end of the ducutus arteriosus. An angle of less than 30° between the vessel and the Doppler beam was accepted for analysis. Three consecutive Doppler velocity waveforms were analyzed and their mean values of were used for analysis (Fig 1). Assessment of fetal AoI Doppler parameters were peak systolic velocity (PSV), end-diastolic velocity (EDV), times-averaged maximum velocities (TAMXV), pulsatility index (PI), and resistance index (RI).
Recordings were performed during the absence of fetal movement. Furthermore, a qualitative assessment of AoI flow, according to the direction of the diastolic flow in the AoI (i.e., antegrade and retrograde flow) was made and used for analysis of perinatal outcomes of each fetus. We did not measure the isthmic flow index (IFI). One experienced operators have performed all the Doppler measurements.
The perinatal outcome included birth-weight, intertwin discordance, and the Apgar score at 5 minutes. Statistical analysis was performed using SPSS ver. 17.0 (SPSS Inc., Chicago, IL, USA). Descriptive statistics were computed for all variables considered in this study. Doppler variables and perinatal outcome were analyzed by Student's t-test, Fisher's exact test and Mann-Whitney test as indicated. The AoI blood flow and other Doppler parameters in predicting adverse perinatal outcomes were assessed by two-way ANOVA test and logistic regression analysis. Statistical significance was assumed at P<0.05.
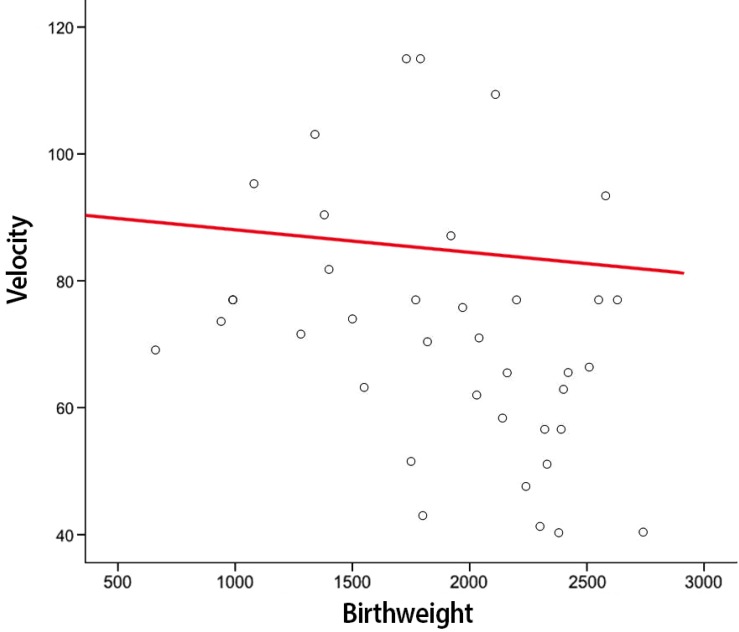
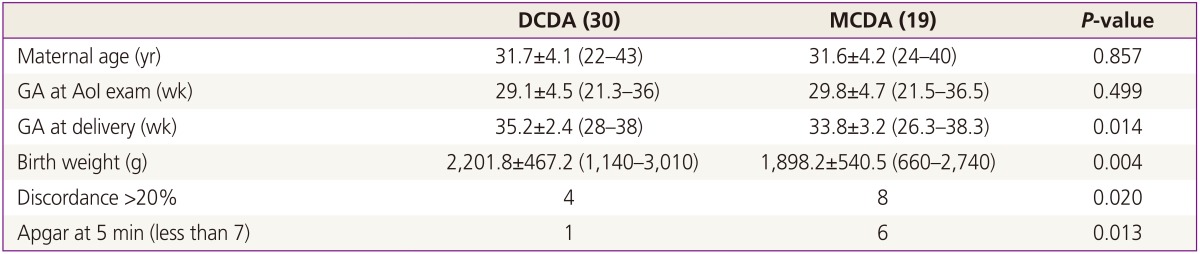
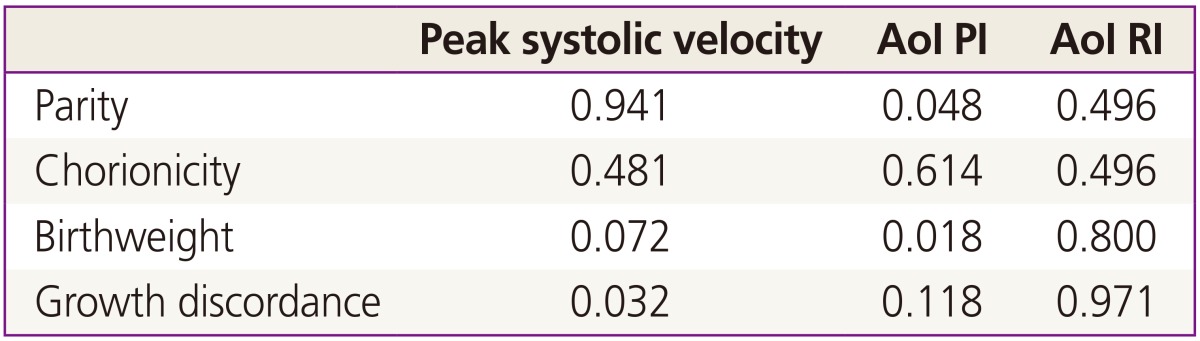
Reliable flow velocity waveforms of the AoI for optimal analysis were obtained in both twin fetuses. The mean maternal age in the study group was 31.7±4.1 years old and the median gestational age was 29.4 weeks (range, 21.3 to 36.5 weeks) at the time of the scan. Gestational weeks at delivery, as well as birth weight were significantly lower in monochorionic twins. The incidence of growth discordance over 20% or more was double in monochorionic twin than that of dichorionic twin. The number of lower Apgar scores at 5 minutes was also shown more commonly in monochorionic twins (Table 1). The PSV, EDV, and TAMXV value did not differ between larger fetus and smaller fetus. However, the AoI PI and RI were significantly higher in smaller fetus than in larger fetus regardless of chorionicity (Table 2). Retrograde flow was noted in five of 55 cases (9.1%) in dichorionic twin and in three of 35 cases (8.6%) in monochorionic twins. There were no significant differences between the chorionicity. The only one case out of total 8 cases was of the larger fetus, while the others were of smaller fetuses. In two-way ANOVA, two significant correlations were found between the AoI PI and birthweight (P=0.018) and between the PSV and growth discordance (P=0.032) (Table 3). In monochorionic twin, a linear correlation between the AoI PI and birthweight (P=0.004) and between AoI PI and growth discordance (P=0.031). Also, there was a meaningful correlation between the PSV and birthweight (P=0.036); identified by the logistic regression analyses (Figs. 2,3,4).
The AoI is the only arterial connection between the right ventricle and the left ventricle. This means that the AoI blood flow pattern reflects the balance between ventricular outputs and provides the evidence for the differences in vascular impedance in either placental or cerebral vascular system [1,8,9]. Therefore, the AoI blood pattern may act as a reliable indicator of the progression of fetal hemodynamic deterioration in fetus. Intrauterine growth restriction (IUGR), especially when it includes the smaller twin fetus of discordant growth, increases the risk of adverse pregnancy outcome. Since there is no effective fetal therapy for IUGR, the timing of delivery is the key issue in the management of affected fetuses.
With the necessity of valuable monitoring of the optimal time for delivery, Doppler parameter was introduced. Umbilical (UmA) and MCA Doppler findings seem to become abnormal in early stages of placental insufficiency. In contrast, DV flow abnormalities have been described as a late marker, since this occurs within the last week before delivery reflecting adverse perinatal outcome and neurological damage [10,11,12,13]. However, there is a gap of some weeks between early and late signs, during which new parameters are needed for better documentation of fetal deterioration. Specifically, Figueras et al. [14] reported that abnormal UmA PI and MCA PI (i.e., outside the 5th to 95th centile range) showed an almost linear deterioration throughout monitoring of IUGR fetus. Such correlation was shown on average 20 days before delivery. Further, the AoI PI became abnormal on average 13 days before delivery, and 7 days for the DV PI.
Due to its closeness to the heart, the Doppler pattern of the AoI was very pulsatile and showed high systolic and low diastolic velocities than that of the MCA and UmA [15]. With advancing gestation, there were significant increase in the PSV, TAMXV, and the PI of the AoI; whereas the RI and EDV of the AoI remained constant during the second half of pregnancy [16].
Our study did not follow the measure of the AoI Doppler flow throughout the entire gestation of twins. Instead, we have measured the AoI PI and RI at on average of 29.4 weeks and the high AoI RI value was observed in smaller twin fetus than in larger twin fetus. Given the 9% average weight difference between the twin fetuses from our results, the high value of AoI PI on smaller fetus could be seen as the effect of the placental vascular resistance, rather than the gestational age.
Ruskamp et al. [17] has described a semiquantitative parameter called the IFI, which is particularly sensitive to the change in both amount and direction of diastolic flow. The IFI is an improved yet still an imperfect index as it involves the manual calculations. For this reason, we did not apply the IFI in our study. Doppler blood flow measurements across the fetal AoI can be reliably obtained from both three vessels view and the traditional long-axis view [18]. In our study, the AoI values have been taken according to the traditional long-axis method. The small diameter of the AoI precludes measurement of actual blood flow volume and so using PI, which is likely to be the best index to assess blood flow through fetal vessels. Indeed, the PI is angle-independent and analyzes blood flow over time taking into account downstream impedance during the whole cardiac cycles. These characteristics suggest that the PI is a useful dictator of fetal hemodynamic changes throughout pregnancy [19,20]. In our results, the birthweight was significantly correlated with AoI PI but not with AoI RI. Since our study is to investigate the characteristics AoI flow of both twin fetuses, we did not perform to measure the umbilical artery and MCA Doppler flow in all cases. We also did not used clinical decision for intervention of smaller fetus of twin by AoI flow. In 7 cases of our study, the absent and reversed flow in umbilical artery was not shown in the retrograde AoI flow of smaller twin.
In placental insufficiency, an increase in placental vascular resistance may change the fetal AoI blood flow profile prior to any significant change in umbilical artery blood pattern [20,21]. The cerebral vasodilatation together with the increase in downstream vascular impedance appears to be the main factors accounting for the decrease of absolute velocities in the AoI.
Decreased blood flow velocity in the AoI was observed in virtually all cases with IUGR. This suggests that this is an early event in the fetal response to placental insufficiency, rather than a late event in the hemodynamic deterioration of such fetuses. Moreover, this low blood flow velocity was often associated with increased afterload of the fetal heart leading to a rise in ventricular pressure and wall tension. This may further increase oxygen demand of the myocardium. This is supported by the fact that fetuses with retrograde net blood flow of the AoI were delivered more frequently by cesarean section due to fetal distress [22]. But in our twin data, we did not have to classify to IUGR in twins. We had divided to larger fetus and smaller one in twins. And we investigated AoI values to predict growth discordance between fetuses. Our results were revealed that birthweight were negatively correlated with both the PSV in AoI flow and the AoI PI. We also observed a positive correlation between AoI PI and the growth discordance ratio in both fetuses. This relationship between the AoI PI and growth discordance possibly explains the effects of AoI PI in smaller fetus [23]. And such relationship between AoI PI and the growth discordance is limited to smaller fetus of monochorionic twin. In monochorionic twin, there are more abundant systemic blood volumes than those in singleton and well develop intertwin vascular anastomoses. There are some presumptions in the case where one of the twins has a normal growth, its blood shifts to the other fetus and maintains the AoI blood stream. As the twins share the placenta, pregnant woman's absolute blood volume is greater than the fetal weight and allows maintaining the AoI blood stream. Further study using data collection and follow up will be needed.
On the basis of our observation, AoI PI in twin was revealed their hemodynamic status and this result may improve the understanding of the growth discordance development. There were revealed the smaller fetus had high AoI PI values regardless to chorionicity and the effects of AoI flow were reflected more prominent in monochorion. These findings might be explained twin hemodynamics and fetal growth in utero.
In conclusion, AoI flow might be meaningful to predict growth discordance in twin at least 4 weeks before delivery.
Acknowledgments
This work was supported by Korean Society of Ultrasound in Obstetrics and Gynecology Research Fund (2008).
References
1. Fouron JC. The unrecognized physiological and clinical significance of the fetal aortic isthmus. Ultrasound Obstet Gynecol 2003;22:441-447. PMID: 14618654.


2. Baschat AA. Fetal responses to placental insufficiency: an update. BJOG 2004;111:1031-1041. PMID: 15383103.


3. Bilardo CM, Wolf H, Stigter RH, Ville Y, Baez E, Visser GH, et al. Relationship between monitoring parameters and perinatal outcome in severe, early intrauterine growth restriction. Ultrasound Obstet Gynecol 2004;23:119-125. PMID: 14770389.


4. Eronen M, Kari A, Pesonen E, Kaaja R, Wallgren EI, Hallman M. Value of absent or retrograde end-diastolic flow in fetal aorta and umbilical artery as a predictor of perinatal outcome in pregnancy-induced hypertension. Acta Paediatr 1993;82:919-924. PMID: 8111171.


5. Eberle AM, Levesque D, Vintzileos AM, Egan JF, Tsapanos V, Salafia CM. Placental pathology in discordant twins. Am J Obstet Gynecol 1993;169:931-935. PMID: 8238151.


6. Weissman A, Achiron R, Lipitz S, Blickstein I, Mashiach S. The first-trimester growth-discordant twin: an ominous prenatal finding. Obstet Gynecol 1994;84:110-114. PMID: 8008303.

7. Benirschke K. Intrauterine death of a twin: mechanisms, implications for surviving twin, and placental pathology. Semin Diagn Pathol 1993;10:222-231. PMID: 8210773.

8. Fouron JC, Skoll A, Sonesson SE, Pfizenmaier M, Jaeggi E, Lessard M. Relationship between flow through the fetal aortic isthmus and cerebral oxygenation during acute placental circulatory insufficiency in ovine fetuses. Am J Obstet Gynecol 1999;181(5 Pt 1):1102-1107. PMID: 10561626.


9. Makikallio K, Jouppila P, Rasanen J. Retrograde aortic isthmus net blood flow and human fetal cardiac function in placental insufficiency. Ultrasound Obstet Gynecol 2003;22:351-357. PMID: 14528469.



10. Baschat AA, Gembruch U, Harman CR. The sequence of changes in Doppler and biophysical parameters as severe fetal growth restriction worsens. Ultrasound Obstet Gynecol 2001;18:571-577. PMID: 11844191.



11. Cosmi E, Ambrosini G, D'Antona D, Saccardi C, Mari G. Doppler, cardiotocography, and biophysical profile changes in growth-restricted fetuses. Obstet Gynecol 2005;106:1240-1245. PMID: 16319247.


12. Ferrazzi E, Bozzo M, Rigano S, Bellotti M, Morabito A, Pardi G, et al. Temporal sequence of abnormal Doppler changes in the peripheral and central circulatory systems of the severely growth-restricted fetus. Ultrasound Obstet Gynecol 2002;19:140-146. PMID: 11876805.


13. Hecher K, Bilardo CM, Stigter RH, Ville Y, Hackeloer BJ, Kok HJ, et al. Monitoring of fetuses with intrauterine growth restriction: a longitudinal study. Ultrasound Obstet Gynecol 2001;18:564-570. PMID: 11844190.



14. Figueras F, Benavides A, Del Rio M, Crispi F, Eixarch E, Martinez JM, et al. Monitoring of fetuses with intrauterine growth restriction: longitudinal changes in ductus venosus and aortic isthmus flow. Ultrasound Obstet Gynecol 2009;33:39-43. PMID: 19115231.


15. Allen LD, Hornberger LK, Sharlanf GK. Normal fetal heart: pulsed Doppler. In: Allen LD, Hornberger LK, Sharlanf GK, editors. Textbook of fetal cardiology. London: Greenwich Medical Media Limited; 2000. p. 81-89.
16. Del Rio M, Martinez JM, Figueras F, Lopez M, Palacio M, Gomez O, et al. Reference ranges for Doppler parameters of the fetal aortic isthmus during the second half of pregnancy. Ultrasound Obstet Gynecol 2006;28:71-76. PMID: 16795125.


17. Ruskamp J, Fouron JC, Gosselin J, Raboisson MJ, Infante-Rivard C, Proulx F. Reference values for an index of fetal aortic isthmus blood flow during the second half of pregnancy. Ultrasound Obstet Gynecol 2003;21:441-444. PMID: 12768553.



18. Del Rio M, Martinez JM, Figueras F, Bennasar M, Palacio M, Gomez O, et al. Doppler assessment of fetal aortic isthmus blood flow in two different sonographic planes during the second half of gestation. Ultrasound Obstet Gynecol 2005;26:170-174. PMID: 16041679.


19. Gosling RG, King DH. Ultrasonic angiology. In: Marcus AW, Adamson L, editors. Arteries and vein. Edinburgh: Churchill Livingstone; 1975. p. 61-98.
20. Bonnin P, Fouron JC, Teyssier G, Sonesson SE, Skoll A. Quantitative assessment of circulatory changes in the fetal aortic isthmus during progressive increase of resistance to umbilical blood flow. Circulation 1993;88:216-222. PMID: 8319336.


21. Sonesson SE, Fouron JC. Doppler velocimetry of the aortic isthmus in human fetuses with abnormal velocity waveforms in the umbilical artery. Ultrasound Obstet Gynecol 1997;10:107-111. PMID: 9286019.



22. Rizzo G, Capponi A, Rinaldo D, Arduini D, Romanini C. Ventricular ejection force in growth-retarded fetuses. Ultrasound Obstet Gynecol 1995;5:247-255. PMID: 7600206.


23. Del Rio M, Martinez JM, Figueras F, Bennasar M, Olivella A, Palacio M, et al. Doppler assessment of the aortic isthmus and perinatal outcome in preterm fetuses with severe intrauterine growth restriction. Ultrasound Obstet Gynecol 2008;31:41-47. PMID: 18157796.


Fig. 3
The correlation between aortic isthmus pulsatility index (Aol PI) and birthweight in monochorionic twin.
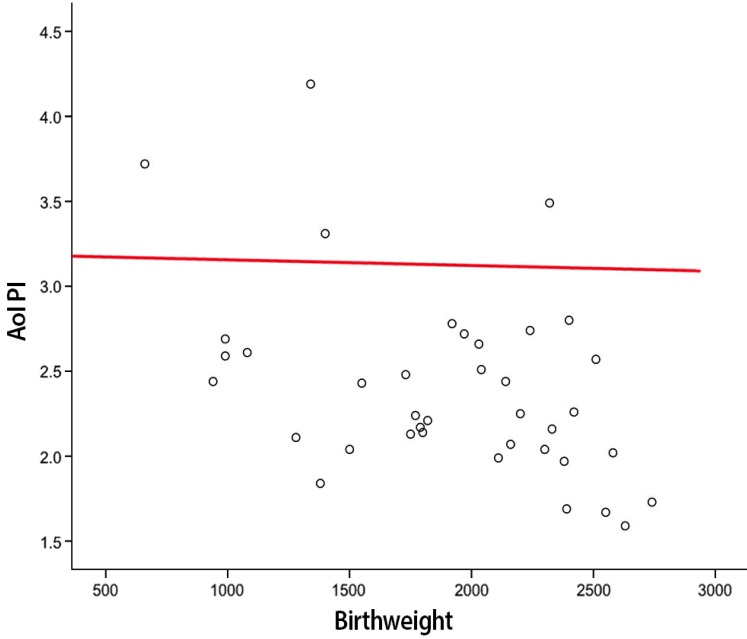
Fig. 4
The correlation between aortic isthmus pulsatility index (Aol PI) and growth discordance in monochorionic twin.
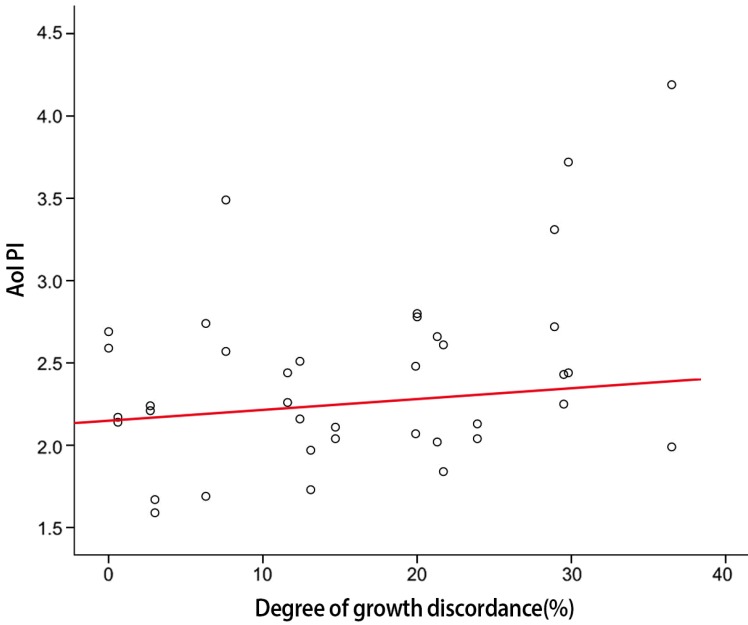
Table 2
Doppler flow for PSV, EDV, TAMXV, AoI PI and RI between larger and smaller fetus by chorionicity
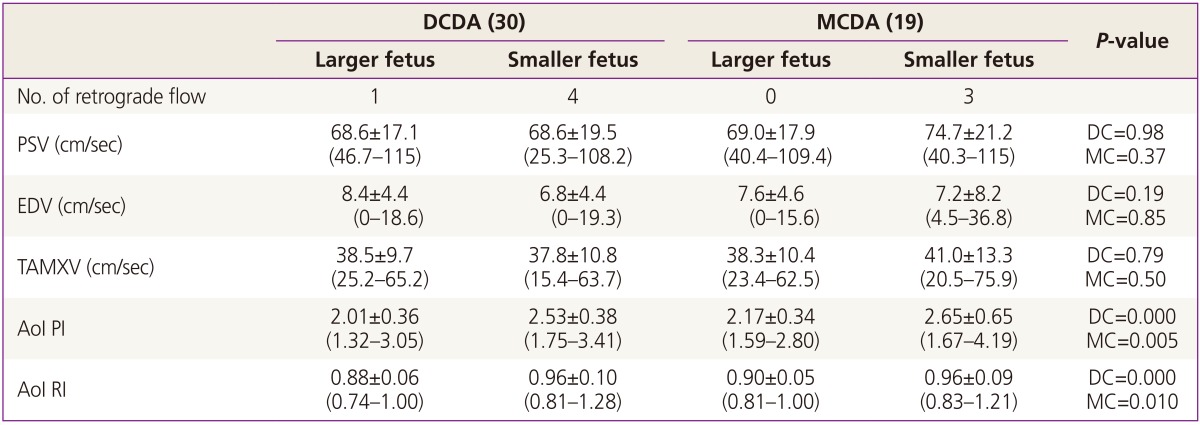
Values are presented as number or mean±standard deviation (range).
PSV, peak systolic velocity; EDC, end diastolic velocity; TAMXV, time average maximum velocity; AoI PI, aortic isthmic pulsatile index; AoI RI, aortic isthmic resistance index; DCDA, dichorionic diamnion; MCDA, monochorionic diamnion.
-
METRICS

-
- 0 Crossref
- 3,316 View
- 19 Download
- Related articles in Obstet Gynecol Sci
-
First reported case of fetal aortic valvuloplasty in Asia2017 January;60(1)