 |
 |
- Search
| Obstet Gynecol Sci > Volume 57(6); 2014 > Article |
Abstract
Leiomyomas are common benign uterine tumors. However, the incidence of vaginal myoma is very rare and may be confused with a variety of vaginal tumors. We report a case of 43-year-old nulligravida who presented with a protruding painful vaginal mass for 7 days. The mass had initially appeared 3 years prior, as 2 to 3 cm that had not subsequently increased. However suddenly, there was rapid severe enlargement over the course of 7 days. Physical exam revealed a monstrous shaped, black color with focal necrosis, odorous protruding vaginal mass about 7 cm in size. The vaginal mass was infected and degenerated. And vaginal wall was also destroyed by the enlarged mass. Because of the clinical features and radiologic findings, the preoperative diagnosis was a vaginal malignancy. We reported an extremely rare case of vaginal myoma that had several characteristics of malignancy, with a brief review of the literature.
Vaginal leiomyoma is a rare tumor, with 300 cases reported in the worldwide literature and seldom in Korea [1]. Though the clinical presentation varies considerably, the tumors are generally small and usually arise along the anterior vaginal wall and rarely in the lateral wall [2]. The tumors are often asymptomatic, but depending on the site of occurrence, they show variable symptoms including lower abdominal pain, low back pain, vaginal bleeding, dyspareunia, urinary symptoms like frequency, dysuria, or other features of urinary obstruction [3]. These lesions can be misdiagnosed as cystocele, urethrocele, skene duct abscess, gartner duct cysts, urethral diverticulum, vaginal cysts, bartholin gland cysts, and vaginal malignancies [4].
This report described the clinical characteristics and radiologic findings of an unusual vaginal leiomyoma, and provided information that can help the clinician to identify such vaginal leiomyomas.
A 43-year-old female patient was treated for a vaginal mass which had been palpable 3 years prior, and recently increased in size over the course of 7 days. The mass had appeared initially 3 years ago as 2 to 3 cm, with no subsequent increases. Sudden, rapid growth occurred during the course of 7 days. She presented at our hospital, with a 7-cm protruding vaginal mass.
The patient was single, nulligravida and her vital sign was not stable with fever (37.9Ōäā). Laboratory evaluation including hematologic, urinary, and routine chemistry tests revealed anemia (hemoglobin 9.5 g/dL) and leukocytosis (white blood cell count 12,000/mL). Tumor marker carbohydrate antigen 125 was within normal limits (11.06 mg/m). Erythrocyte sedimentation rate and C-reactive protein were elevated (55 mm/hr and 12.57 mg/dL). She complained of sharp pain in the perineal area, a sense of dragging down and odorous smell since 7 days prior. On vaginal examination, an irregular shaped tender protruding vaginal mass, black color with multiple focal necrosis, was found in the anterior wall of the vagina, proximal to the urethral orifice. Fig. 1 demonstrated the external appearance at the time of surgery. Initially the origin of the vaginal mass was not obvious. It was thought to arise from the anterior vaginal wall or bladder. The vaginal wall was destroyed and ruptured by the vaginal mass, hence half the vaginal mass was exposed, uncovered by vaginal wall. The cervix, uterus and adnexal regions were unremarkable.
Transvaginal ultrasonography revealed a 7-cm-sized solid mass at the anterior aspect of the vagina. It was intimately related to the vagina, with poor visualization of the vaginal stripe. The uterus was normal. Abdominopelvic computed tomography (CT) was performed, demonstrating a 5.5-cm-sized perineal tumor, and several reactive inguinal lymph nodes. These were not classified to be originating from the vaginal mass. Hence we performed pelvic magnetic resonance imaging (MRI) that clarified a mass of 7├Ś5 cm at the distal end left anterior aspect of the vagina, displacing the urethra anteriorly. It had low signal intensity on T1-weighted image, high signal intensity on T2-weighted image, and irregular enhancement on post-contrast enhanced image as if it were a malignant tumor (Fig. 2). There were several tiny intramural and subserosal myomas in the uterus. Bilateral fallopian tubes and ovaries had unremarkable findings. Punch biopsy of the vaginal mass revealed granulation tissue. The preoperative diagnosis was vaginal malignancy.
Because of its infected status, we used antibiotics for 10 days before the surgery. Under general anesthesia, the patient underwent excision of the mass through a vaginal approach without opening the urinary tract.
Grossly there was a relatively circumscribed mass measuring 8├Ś7.3├Ś4.5 cm of which the cut surface was pale tan colored and firm solid in consistency. The luminal surface was ulcerated. Microscopic examination revealed a well circumscribed tumor lesion composed of interlacing fascicles of spindles cells which were diffusely positive for smooth muscle actin (Fig. 1B).
After surgery, a Foley catheter was left in place for 6 days, with normal voiding resumed after its removal. The patient was discharged on postoperative seven day without any complication.
Vaginal leiomyoma is a rare tumor, with 300 cases reported in the world literature and also seldom in Korea [1]. Leiomyomas in the vagina are mostly common encountered in the age range of 35 to 50 years [4]. They usually arise in the anterior wall but may be found in any location. Vaginal leiomyomas are generally moderately firm, but as they may undergo degenerative changes, as occurs in the uterus, they may vary in consistency from firm to soft [5]. They generally vary in size from 1 to 5 cm in diameter, and may or may not be pedunculated and covered mostly with smooth intact vaginal mucosa. They usually are asymptomatic until they reach a certain size (usually Ōēź6 cm) [6]. Liu [6] analyzed 11 vaginal leiomyomas, and their average time to be show symptomatic was 8.4 years. Depending on the site of occurrence, they show variable symptoms including lower abdominal pain, low back pain, vaginal bleeding, dyspareunia, urinary symptoms like frequency, dysuria, or other features of urinary obstruction [3]. In this case, the patient had perineal pain, and a sense of dragging down due to vaginal mass. The mass was about 7 cm in diameter, with accompanied necrosis of the overlying vaginal mucosa, purulent discharge, and bleeding on touch. The vaginal mass had a degenerated and infected status, and the patient was febrile.
The diagnosis was made through transvaginal ultrasonography, abdominopelvic CT, pelvic MRI, and punch biopsy. MRI especially provides useful preoperative information about the morphological and structural characteristics of the mass and the anatomical relationship between the lesion [7]. A vaginal leiomyoma generally has low signal intensity on T1-weighted images similar to surrounding muscles and still relatively low signal intensity on T2-weighted images [7,8,9]. They are typically rounded, well circumscribed, whorled appearing masses. Other vaginal tumors, such as a carcinoma, invasive cervical carcinoma and rhabdomyosarcoma, have a different appearance on MRI. They generally have higher signal intensity on T2 images with irregular margins and most are heterogenous enhanced after gadolinium administration due to the presence of areas of necrosis or hemorrhage [8]. On MRI, a high signal intensity lesion with heterogeneity on T2-weighted images and an irregular enhancement on post contrast enhanced images should raise the concern of vaginal tumors such as a leiomyosarcma and rhabdomyosarcoma. Degenerated leiomyomas can also show foci of high signal intensity that correspond to a combination of edematous swelling of myoma cells from ischemia, cystic change, and/or myxoid degeneration [10]. In our case, the mass had grossly rugged and aggressive features.
The differential diagnosis of vaginal mass includes cystocele, urethrocele, skene duct abscess, gartner duct cyst, urethral diverticulum, vaginal cyst, bartholin gland cyst, epidermal inclusion cyst and a variety of both benign and malignant vaginal tumors [4]. In our case, the vaginal mass was grossly irregular in shape combined with necrotic foci, and had grown rapidly. The vaginal wall mucosa was also broken. Secondary features such as rapid growth, an infiltrative nature and presence of metastasis are useful tips for distinguishing leiomyosarcoma from benign entities [11]. Vaginal leiomyoma, especially the borderline variety may undergo sarcomatous change [12]. Liu [6] reported an incidence of 9.1% for malignant change. In a retrospective analysis of leiomyosarcomas, malignant transformation was more common in extra-uterine leiomyomas [11]. Traumatic stimuli of the tumor could increase mitotic activity [13]. It was observed that pedunculated submucosal myomas are subjected to greater stimuli and are associated with increased mitotic activity [13]. Interestingly a case was reported with 91% of vaginal leiomyosarcoma covered with healthy, intact vaginal mucosa which did not extend beyond the primary mass, however, in an advanced stage at the time of presentation, the vaginal leiomyosarcoma was already a friable, ulcerated, exophytic mass [14]. Although the final diagnosis was a vaginal leiomyoma in our case, taking into account the clinical features and MRI images of the case, the clinical course could have progressed from a vaginal leiomyoma to a degenerated leiomyoma. The change might to be considered to have progressed to vaginal sarcoma.
Surgery through the vaginal route has been reported as the treatment of choice. If a vaginal mass is located at the anterior vaginal wall, urethral catheter insertion is helpful to prevent urethral injury [6]. Recurrence of the tumor is a serious consideration, hence the patient needs to be followed up.
In Korea, few cases of vaginal leiomyoma were reported. Most of the cases had ordinary features of vaginal myoma. Only one case was reported with malignant radiologic findings, however, the case had clinically benign nature [15]. Thus, there is no report about vaginal myoma that had radiologic and clinical characteristics which similar to the malignancy up to date. Our case had an unusual presentation compared to vaginal leiomyoma reported before. We described this rare case with a brief review of literature.
References
1. Young SB, Rose PG, Reuter KL. Vaginal fibromyomata: two cases with preoperative assessment, resection, and reconstruction. Obstet Gynecol 1991;78:972-974. PMID: 1923243.

2. Freed SZ, Haleem SA, Wiener I, Feldman J. Bladder outlet obstruction caused by vaginal fibromyoma: the female prostate. J Urol 1975;113:30-31. PMID: 46288.


5. Oruc S, Karaer O, Kurtul O. Coexistence of a prolapsed, pedunculated cervical myoma and pregnancy complications: a case report. J Reprod Med 2004;49:575-577. PMID: 15305833.

6. Liu MM. Fibromyoma of the vagina. Eur J Obstet Gynecol Reprod Biol 1988;29:321-328. PMID: 3229545.


7. Pavlica P, Bartolone A, Gaudiano C, Barozzi L. Female paraurethral leiomyoma: ultrasonographic and magnetic resonance imaging findings. Acta Radiol 2004;45:796-798. PMID: 15624526.


8. Shadbolt CL, Coakley FV, Qayyum A, Donat SM. MRI of vaginal leiomyomas. J Comput Assist Tomogr 2001;25:355-357. PMID: 11351183.


9. Ikeda R, Suga K, Suzuki K. MRI appearance of a leiomyoma of the female urethra. Clin Radiol 2001;56:76-79. PMID: 11162704.


10. Siegelman ES, Outwater EK. Tissue characterization in the female pelvis by means of MR imaging. Radiology 1999;212:5-18. PMID: 10405714.


11. Hubert KC, Remer EM, Rackley RR, Goldman HB. Clinical and magnetic resonance imaging characteristics of vaginal and paraurethral leiomyomas: can they be diagnosed before surgery? BJU Int 2010;105:1686-1688. PMID: 19889060.


12. Cobanoglu O, Gurkan Zorlu C, Ergun Y, Kutluay L. Leiomyosarcoma of the vagina. Eur J Obstet Gynecol Reprod Biol 1996;70:205-207. PMID: 9119105.


13. Haque AU, Moatasim A, Aslam F. Mitotically active leiomyoma: a word of caution. Int J Pathol 2004;2:38-41.
14. Ahram J, Lemus R, Schiavello HJ. Leiomyosarcoma of the vagina: case report and literature review. Int J Gynecol Cancer 2006;16:884-891. PMID: 16681778.


15. Suh DH, Lim SY, Chung J, Choi HJ, Lee S, Park SY. Vaginal leiomyoma mimicking a malignant neoplasm on MR imaging. Korean J Obstet Gynecol 2006;49:2432-2437.
Fig.┬Ā1
(A) An irregular shaped tender protruding vaginal mass, black color with multiple focal necrosis, was found. The vagina mucosa was broken (arrows). (B) The high power photogram demonstrated the bundles of spindle cells interlacing in right angle. There was less than 2 mitotic figure (H&E, ├Ś200).
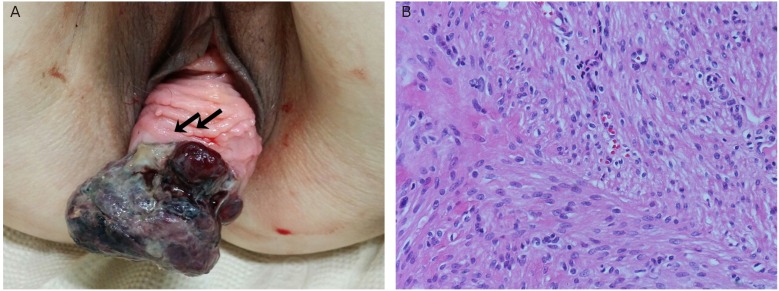
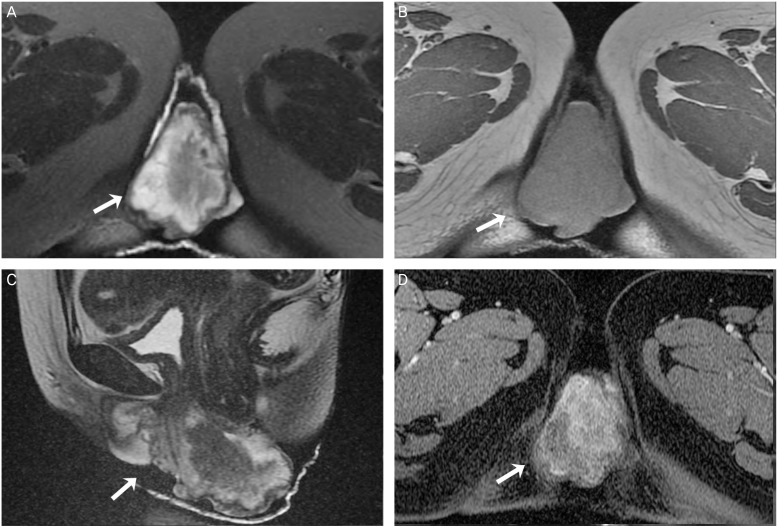
Fig.┬Ā2
Vaginal mass in a 43-year-old woman. (A) T2-weighted axial magnetic resonance (MR) image shows irregular shaped mass (arrow) in the vagina. The signal intensity of the mass is heterogenous and higher compared that of pelvic muscle. (B) T1-weighted axial MR image. The signal intensity of the mass (arrow) is similar to that of pelvic muscle. (C) The mass (arrow) has heterogenous high signal intensity on T2-weighted sagittal MR image. (D) The mass (arrow) has irregular enhancement on contrast enhanced T1-weighted MR image
-
METRICS

-
- 12 Crossref
- 3,618 View
- 27 Download
- Related articles in Obstet Gynecol Sci
-
Vaginal leiomyoma mimicking a malignant neoplasm on MR imaging.2006 November;49(11)
Tamoxifen-associated polypoid endometriosis mimicking an ovarian neoplasm2015 July;58(4)



















