 |
 |
- Search
| Obstet Gynecol Sci > Volume 65(4); 2022 > Article |
|
Abstract
Objective
Methods
Results
Acknowledgements
Notes
Ethical approval
The study protocol was approved by the Siriraj Institutional Review Board (SIRB) of the Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand (COA No. Si 060/2017).
Patient consent
All study participants provided written informed consent prior to enrollment. However, the use of images from patients are not required for the publication.
Author contributions
Nida Jareemit: Conceptualization, methodology, formal analysis, data curation, writing-original draft, writing-review and editing
Navin Horthongkham: Writing-review and editing
Suwanit Therasakvichya: Writing-review and editing
Boonlert Viriyapak: Writing-review and editing
Perapong Inthasorn: Writing-review and editing
Mongkol Benjapibal: Writing-review and editing
Vuthinun Achariyapota: Writing-review and editin
Irene Ruengkhachorn: Conceptualization, methodology, writing-review and editing
Fig. 1
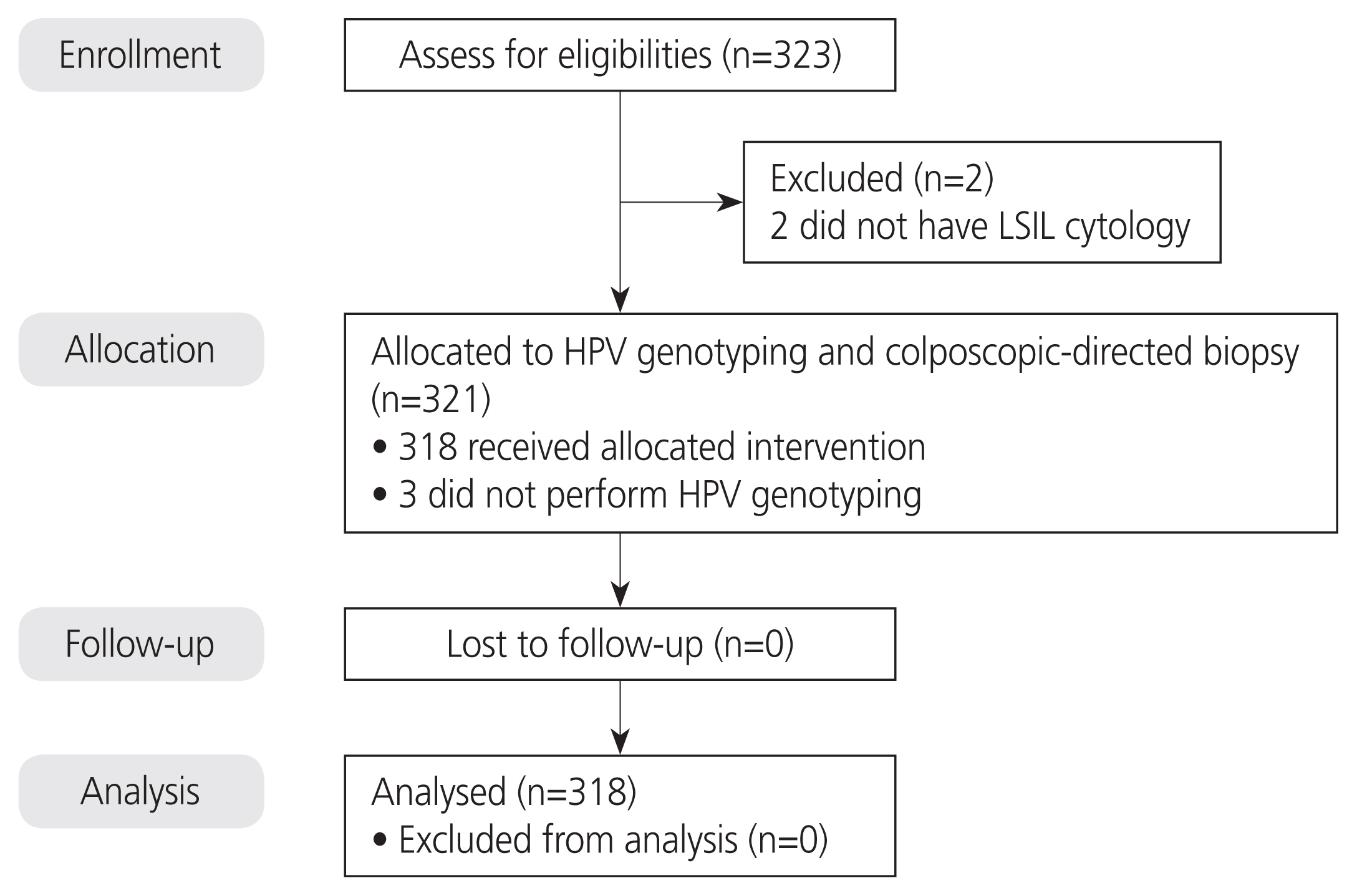
Fig. 2
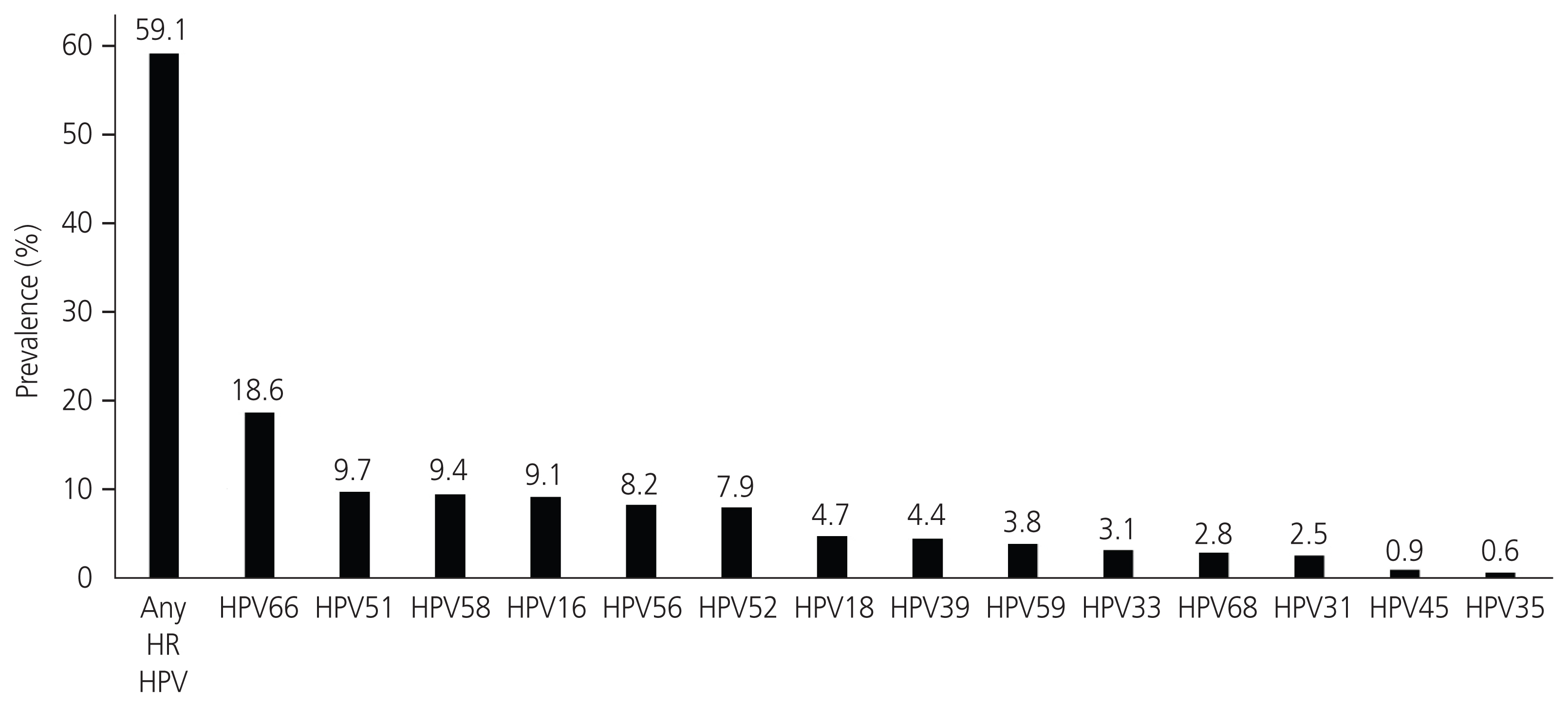
Table 1
Table 2
Table 3
| Type of HPV testing | Number of colposcopies | Sensitivity (% [95%CI]) | Specificity (% [95%CI]) | PPV(% [95%CI]) | NPV(% [95%CI]) | AUROC |
|---|---|---|---|---|---|---|
| No HPV testing | 318 (100.0) | |||||
| HPV testinga) | 188 (59.1) | 78.9 (53.9-93) | 42.1 (36.5-47.9) | 8 (4.7-13) | 96.9 (91.8-99) | 0.60 (0.5-0.7) |
| Partial HPV genotypingb) | 42 (13.2) | 10.5 (1.3-33.1) | 95.2 (92-97.4) | 13.3 (1.7-40.5) | 93.8 (90.3-96.4) | 0.53 (0.5-0.6) |
| HPV genotypingc) | 142 (44.7) | 31.6 (12.6-56.6) | 59.9 (53.8-65.8) | 5.2 (1.9-11) | 92.6 (87.7-96) | 0.46 (0.35-0.57) |
| P-value | <0.001 | 0.149 |
CIN2+, cervical intraepithelial neoplasia 2 or higher lesion; HPV, human papillomavirus; CI, confidence interval; PPV, positive predictive value; NPV, negative predictive value; AUROC, area under the receiver operating characteristic curve.
a) HPV testing was reported using two categories; negative 14 high-risk HPV or positive any of 14 high-risk HPV (16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 66, and/or 68);
Table 4
| Variable | LSIL histology (n=299) | HSIL histology (n=19) | P-value |
|---|---|---|---|
| Age (yr) | 0.649 | ||
| <30 | 57 (96.6) | 2 (3.4) | |
| 30-49 | 193 (93.7) | 13 (6.3) | |
| ≥50 | 49 (92.5) | 4 (7.5) | |
| Menopause status | 0.132 | ||
| Pre-menopause | 269 (94.7) | 15 (5.3) | |
| Menopause | 30 (88.2) | 4 (11.8) | |
| Prior abnormal screening | 0.790 | ||
| No or unknown | 221 (93.6) | 15 (6.4) | |
| Yes | 78 (95.1) | 4 (4.9) | |
| Colposcopic finding | 0.028a) | ||
| Normal or low-grade lesion | 282 (94.9) | 15 (5.1) | |
| High-grade lesion or cancer | 17 (81.0) | 4 (19.0) | |
| HPV genotype | 0.097 | ||
| Negative | 126 (96.9) | 4 (3.1) | |
| Positive HPV non-16/18 | 58 (19.4) | 7 (36.8) | |
| Positive HPV16/18 | 115 (38.5) | 8 (42.1) | |
| Colposcopic finding with HPV status | <0.001a) | ||
| Low grade lesion with HPV− | 117 (39.1) | 4 (21.1) | |
| High grade lesion with HPV− | 9 (3.0) | 0 | |
| Low grade lesion with HPV+ | 165 (55.2) | 11 (57.9) | |
| High grade lesion with HPV+ | 8 (2.7) | 4 (21.1) | |
| Number of high-risk HPV infections | 0.172 | ||
| No HPV infection | 126 (96.9) | 4 (3.1) | |
| Single infection | 117 (92.1) | 10 (7.9) | |
| Multiple infections | 56 (91.8) | 5 (8.2) |
References
- TOOLS





















